Behavioral health organizations face staffing shortages, burnout, and administrative challenges that disrupt care delivery. Generic HR systems often fail to meet their needs, leading to inefficiencies and compliance risks. Care-focused Human Capital Management (HCM) systems address these issues by automating hiring, scheduling, and payroll processes while simplifying credential tracking and compliance management. These tools streamline operations, reduce burnout, and improve workforce retention.
Key takeaways:
- Hiring: Automates job postings, credential verification, and onboarding workflows, cutting down delays and errors.
- Scheduling: Dynamically matches staff based on qualifications and availability, ensuring compliance with staff-to-client ratios.
- Payroll: Handles complex pay structures and integrates with position control for accurate payments tied to roles and funding.
- Compliance: Tracks licenses, certifications, and regulations, sending automated alerts to avoid lapses.
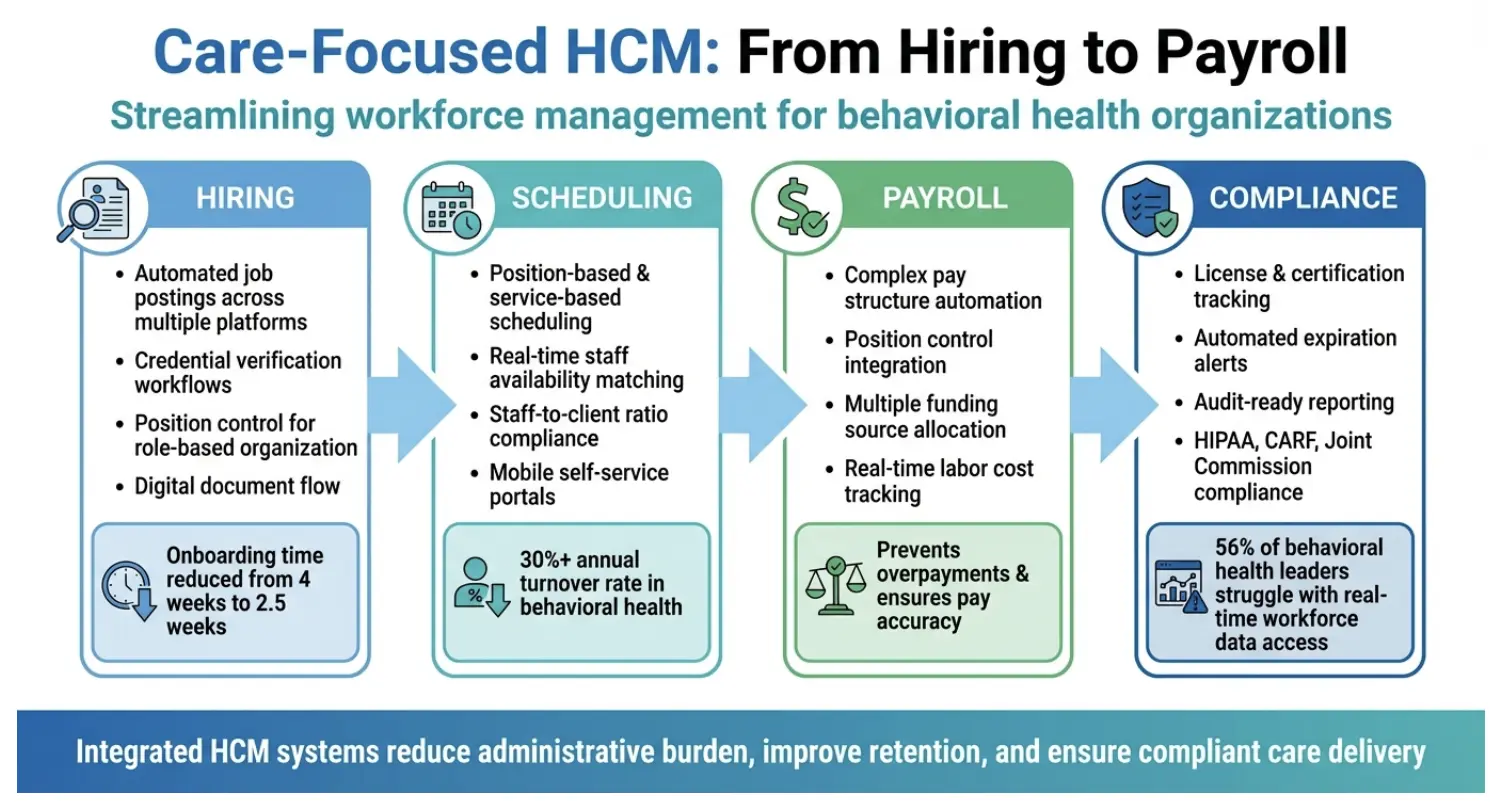
HCM System Workflow for Behavioral Health Organizations: Hiring to Payroll
How HCM Systems Improve Hiring in Care Organizations
Finding and hiring skilled behavioral health professionals is no easy feat, especially with the limited talent pool in the industry. Generic HR software often falls short when it comes to managing the specific credentials and requirements these roles demand.
That’s where HCM systems tailored for care organizations come into play. Unlike traditional HR tools, these systems use position control to organize the workforce by role rather than by individual employees. This approach gives hiring managers a clear, real-time view of vacant positions, role-specific credentials, and salary allocations. One CFO from a non-profit organization shared their experience:
“The position control function of this software is unique to all products we reviewed. It mirrored a manual system we had been using for years to insure financial control and funder compliance.”
– CFO, Non-Profit Organization Management
This level of visibility is crucial, especially since 56% of behavioral health leaders report difficulties accessing workforce data in real time. With this insight, organizations can adopt proactive recruitment strategies, reducing delays and addressing inefficiencies in the hiring process.
Recruitment and Onboarding Tools
Care-focused HCM systems streamline recruitment by enabling one-click job postings across multiple platforms like Indeed, state job boards, and internal career sites. Applications are funneled into a centralized, searchable database, making it easier for teams to collaboratively score and filter candidates.
Onboarding is just as seamless, thanks to automated workflows. These workflows use role-based templates to assign tasks based on the position, department, or location. For instance, a therapist might need to provide CPR certification and a clinical license, while a billing clerk would not. These tailored workflows ensure no steps are missed.
The benefits are clear. Behavioral Progression, Inc. saw onboarding times for therapists drop from four weeks to just 2.5 weeks after replacing manual processes with automated templates. Their HR team completed tasks three times faster, and new hires asked 60% fewer questions. Similarly, All About Kids, a pediatric therapy provider with 1,200 employees, eliminated documentation errors by automating their paper-based system, giving managers full visibility over the hiring process.
Another standout feature is the digital document flow. Onboarding forms automatically populate HR and payroll systems, reducing manual data entry errors that could delay paychecks. Additionally, SLA alerts and escalations help keep critical tasks – like I-9 verification or license uploads – on schedule, ensuring compliance deadlines are met.
These tools not only simplify recruitment but also set the stage for ongoing compliance and quality assurance.
Credential Tracking and Regulatory Requirements
Behavioral health roles often come with stringent credentialing requirements that vary by position, state, and funding source. With a care-specific HCM system, you can define credential requirements by role before posting a job. This allows recruiters to filter candidates upfront, avoiding compliance issues later.
Integrated background checks and credential verification are built directly into the hiring workflow. The system continuously monitors licenses, certifications, and vaccination records, sending automated alerts for expiring credentials to both employees and supervisors. This proactive approach helps organizations stay ahead of compliance audits and site visits.
Enhanced approval workflows also improve communication across teams:
“The functionality of the approval workflow and notification has significantly improved communication across the organization, especially for onboarding.”
– CFO, Non-Profit Organization Management
Digitizing credential verification, policy acknowledgments, and hiring packet collection creates a secure audit trail. This not only protects organizations from compliance risks and fines but also simplifies regulatory reviews by enabling EEO/OFCCP-compliant data collection through role-based permissions.
When HCM systems clearly outline and automatically verify credential requirements, they eliminate costly hiring errors. This ensures every new hire is fully prepared to deliver compliant care from their very first day.
Staff Scheduling for Behavioral Health Organizations
Once you’ve hired the right team, the next hurdle is making sure they’re where they need to be – exactly when they’re needed. Behavioral health organizations run 24/7, meaning schedules often need to shift at a moment’s notice. Whether it’s crisis centers, residential programs, or outpatient services, these settings demand constant coverage. Even a brief staffing gap can ripple into serious consequences for patient care and safety.
Adding to the challenge is the behavioral health sector’s turnover rate, which often exceeds 30% annually. Managers must juggle strict staff-to-client ratios, cover sudden absences, and coordinate across multiple locations. Generic scheduling tools often fall short under such pressure. Below, we’ll explore common scheduling challenges and how specialized HCM systems can address them.
Common Scheduling Problems in Care Settings
One of the biggest hurdles is handling unexpected absences. When a clinician calls out sick or misses a shift, managers scramble to find a qualified replacement. Without a system that provides real-time visibility into staff availability and credentials, these gaps can lead to compliance issues. Worse, remaining staff may be forced to take on extra shifts, increasing the risk of burnout.
Another major issue is compliance with mandated staff-to-client ratios. These ratios vary depending on the type of program and the clients’ needs. Even a temporary lapse can result in fines or jeopardize accreditation. For organizations managing multiple programs or locations, manual scheduling makes it nearly impossible to monitor these ratios in real time.
Then there’s the need for immediate adjustments. A client crisis, an unexpected admission, or a sudden change in acuity can require staffing changes within minutes. Managers need tools that allow them to respond quickly, all while staying compliant with labor laws and credential requirements. This is where care-focused HCM systems come into play, offering dynamic scheduling solutions to tackle these challenges.
Position-Based and Service-Based Scheduling Methods
Specialized HCM systems for behavioral health organizations address these issues through two key approaches: position-based scheduling and service-based scheduling
- Position-based scheduling focuses on predefined roles. Managers set staffing patterns for specific roles – like licensed clinicians, case managers, or support staff – based on care requirements. The system then matches employees to shifts based on their qualifications and availability. This ensures critical roles are always filled while adhering to licensing rules.
- Service-based scheduling allocates staff based on the services or programs being provided. For organizations offering diverse programs like crisis intervention, residential treatment, or outpatient care, this approach allows staffing levels to shift dynamically based on client needs and acuity.
Modern HCM platforms often combine these two methods, giving managers the flexibility to handle both predictable and variable demands. Features like self-service portals let employees view schedules, request time off, swap shifts with qualified colleagues, or pick up extra shifts via a mobile app. This not only fills shifts faster but also gives employees more control over their schedules, which can help reduce turnover and improve satisfaction.
When these scheduling systems integrate with credential tracking and payroll, they ensure only qualified and certified staff are assigned to roles. Real-time alerts notify managers of coverage gaps, potential overtime issues, and upcoming credential expirations. By automating these processes, scheduling becomes a proactive, data-driven task that supports both staff well-being and high-quality patient care.
Payroll Processing and Compliance Management
Once scheduling and credential tracking are streamlined, the focus shifts to payroll processing. For behavioral health organizations, this is no small feat. These workplaces often juggle complex payroll scenarios involving full-time staff, per diem workers, contractors, and grant-funded positions – each with unique pay structures. A single payroll mistake can erode trust, lead to compliance headaches, or throw budgets off balance, jeopardizing financial health.
Traditional payroll systems often struggle in these environments. They typically aren’t equipped to handle the intricacies of care settings, where employees may juggle multiple roles with different pay rates or where labor costs need to be divided among various funding sources. Specialized HCM platforms step in to fill this gap, automating intricate calculations and reducing manual errors, which lowers the risk of costly mistakes.
Payroll Integration with Position Control
Integrating payroll with position control is a game-changer for ensuring pay accuracy. These systems consolidate employee hours, approved roles, and budget constraints into a unified framework . This setup prevents overpayments and ensures employees are paid correctly based on their authorized roles. For example, if a case manager picks up extra per diem crisis shifts, the system automatically applies the correct pay rates. Real-time updates from timekeeping systems also streamline tax and garnishment calculations, while self-service portals give employees instant access to their pay details.
This integration goes beyond individual paychecks. It provides real-time insights into labor costs tied to specific roles or programs. In behavioral health settings, where staffing needs can shift due to client acuity or 24/7 operations, this transparency is invaluable. Detailed reporting helps optimize staffing levels, reducing reliance on high-cost agency workers – a crucial advantage in an industry where turnover rates can soar above 30%.
Labor Law and Licensing Compliance
Compliance with labor laws is non-negotiable in care settings. HCM systems tailored for behavioral health automate adherence to federal and state regulations, handling tasks like tax withholdings, overtime calculations, and garnishment processing. These platforms generate audit-ready reports, ensuring compliance with laws like the Fair Labor Standards Act.
License compliance is equally critical. Many care staff need to maintain multiple state-specific certifications. HCM systems can flag expired licenses and prevent employees from being scheduled or paid until the issue is resolved. Some platforms even integrate with learning management systems, linking required training directly to license renewals. This creates a seamless compliance process, ensuring staff credentials remain up-to-date while reducing administrative burdens. By automating these workflows, organizations can maintain operational efficiency and focus on delivering high-quality care.
Using HCM Analytics to Improve Workforce Performance
HCM analytics turn workforce data into actionable insights that can directly influence staff retention and improve care quality. This is especially crucial in behavioral health settings, where turnover rates often exceed 30%. Modern HCM systems track critical metrics like departmental turnover, overtime usage, onboarding timelines, and engagement patterns in real time. These insights help organizations identify challenges and implement strategic workforce improvements.
Performance Data and Training Programs
HCM analytics play a key role in identifying skill gaps by tracking training completion rates and competency evaluations. For instance, if a department shows high turnover alongside low training completion rates, it can signal the need for mandatory continuing education or HIPAA refreshers. Integrated learning management tools make it easier to assign, monitor, and report on training across multiple locations, with mobile options that cater to field-based staff.
The connection between training efforts and performance outcomes becomes clearer with analytics. For example, organizations can measure how skill-building programs impact onboarding timelines or reduce overtime costs. This demonstrates the tangible benefits of continuous education. Advanced systems even use AI to detect early signs of burnout through pulse surveys and feedback loops. These systems can recommend personalized development plans or wellness modules to address issues like vicarious trauma. By tackling burnout proactively, organizations address one of the main causes of chronic retention problems in the behavioral health sector.
Role-Based Access and Audit Readiness
HCM analytics also enhance workforce management by refining processes like hiring, scheduling, and payroll. Role-based access controls allow managers to focus on department-specific insights, while executives can view broader organizational trends. This ensures both secure data handling and effective workforce planning.
Compliance dashboards provide real-time updates on critical areas like credential tracking, license renewals, and mandatory training. Automated alerts flag issues, such as expired certifications or overdue performance reviews, before they escalate into larger problems. Additionally, secure audit trails create a verifiable history of workforce management, which is essential for regulatory reviews. This setup helps organizations stay compliant with HIPAA, state licensing requirements, Medicaid billing standards, and accreditation standards from bodies like CARF and The Joint Commission.
Conclusion
Running a behavioral health or human services workforce comes with challenges that go far beyond what generic HR software can handle. From managing 24/7 scheduling to juggling complex payroll allocations across multiple funding sources, care organizations operate in a world with unique demands. Add in the need for strict credential tracking and high turnover rates, and the need for specialized solutions becomes clear. That’s where ContinuumCloud‘s DATIS HCM steps in.
ContinuumCloud’s DATIS HCM offers a unified, cloud-based platform tailored specifically for behavioral health organizations. It simplifies the entire employee lifecycle, from recruitment and onboarding to scheduling and payroll, with automated workflows that ease administrative workloads.
The platform excels at handling intricate payroll needs, such as employees working in multiple roles or distributing labor costs across various grants and cost centers. Features like mobile self-service tools not only lighten the HR team’s load but also improve employee satisfaction.
By integrating critical functions like workforce management, clinical documentation through Welligent, and client engagement via CaredFor into one platform, organizations can achieve greater operational efficiency. This streamlined approach enhances care delivery while providing real-time analytics on key metrics like turnover rates, cost-per-hire, and labor utilization. These insights empower organizations to make informed decisions that stabilize their workforce and improve client outcomes.
For behavioral health organizations striving to deliver exceptional care while staying financially sound, investing in an HCM system designed specifically for their needs is a smart move toward long-term success.
FAQs
How can HCM systems designed for care-focused organizations help reduce employee turnover?
These systems also come equipped with tools to enhance employee engagement and streamline every stage of the employee lifecycle. By fostering a supportive and organized work environment, they help reduce burnout, improve job satisfaction, and make it easier to retain skilled professionals.
How does integrating payroll with position control benefit care-focused organizations?
This method also enhances budgeting precision by tying payroll costs directly to specific roles, making it easier to allocate resources efficiently. Beyond that, it simplifies workflows and minimizes administrative hurdles, leading to smoother operations and improved adherence to workforce regulations.
How do HCM systems help care organizations stay compliant with credentialing and regulatory requirements?
By bringing all employee information into one centralized platform and automating compliance checks, these systems cut down on administrative workload and reduce the chances of mistakes. This allows organizations to dedicate more energy to providing excellent care while staying on top of regulatory requirements.




