Behavioral health organizations often face challenges when their EHR systems fail to meet the demands of residential and outpatient care. Outdated systems lead to inefficiencies, lost productivity, and staff frustration. Here are the five main signs your EHR system might be holding you back:
- Workarounds for Residential Programs: Staff rely on manual processes like spreadsheets for tasks such as bed management and medication tracking, leading to errors and inefficiencies.
- Excessive Documentation Time: Clinicians spend up to 55% of their time on documentation, often dealing with systems that don’t support behavioral health workflows, costing clinics time and money.
- Limited Data Visibility: Disconnected systems prevent leadership from accessing real-time insights into capacity, performance, and billing, making informed decisions difficult.
- Scaling Issues: As organizations grow, fragmented systems create inefficiencies, requiring separate software for different programs and complicating data integration.
- Staff Frustration: Inefficient EHRs contribute to burnout, with 60% of behavioral health professionals citing system-related frustrations as a key issue.
These challenges can impact care delivery, staff satisfaction, and financial performance. Modern EHR platforms designed for behavioral health can address these issues by unifying workflows, reducing documentation time, and improving data accessibility.
Your Residential Programs Rely on Workarounds
Residential treatment programs have unique demands that differ significantly from outpatient clinics. Staff need to monitor bed availability in real time, manage large-scale medication administration across shifts, coordinate incident reporting, and maintain accurate census data. When an EHR system isn’t tailored to these specific needs, teams are left to create makeshift solutions. This often means relying on manual workarounds.
These workarounds typically include a mix of spreadsheets, paper logs, and sticky notes to handle essential tasks. For instance, bed availability might be tracked in Excel, medication passes could depend on handwritten records, and incident reports might be scattered across separate documents. Such systems not only lack a clear audit trail for task completion but also make it easy for critical information to slip through the cracks – especially when a patient transitions from detox to residential care. Managing these care journeys requires a system that can automate tasks and check-ins across different levels of care. The result? Disconnected processes that disrupt workflows and introduce unnecessary risks and costs.
These manual systems also waste valuable time and can jeopardize patient care. They highlight the need for an EHR specifically designed to support the demands of residential treatment programs. Generic EHRs, often built for primary care, fall short in several areas. They struggle with high-volume medication management, shift-based task coordination, and the narrative documentation formats – like SOAP, DAP, and BIRP – that are essential in residential behavioral health settings.
When residential staff are forced to manage critical operations outside the EHR, it’s a clear sign the system isn’t meeting their needs. While these workarounds might seem manageable initially, they lead to visibility gaps, increase the likelihood of errors, and pile on administrative burdens that only grow as the organization expands.
Clinicians Spend Too Much Time Documenting Care
Proper documentation is essential, but for many clinicians, it feels like a constant uphill battle. Behavioral health clinicians, for instance, spend a staggering 34%–55% of their time on documentation instead of focusing on patient care and engagement. And the work doesn’t stop when the clinic closes – on average, clinicians dedicate 1.4 hours after hours to EHR tasks, often referred to as “Pajama Time”.
Why is this happening? A big part of the problem lies in systems that just aren’t built with behavioral health workflows in mind. Many EHRs are designed for quick, 15-minute visits with checkbox-style input. But behavioral health sessions, which often last 50 minutes, require detailed narrative documentation using formats like SOAP, DAP, or BIRP. Instead of streamlining the process, these systems force clinicians to manually input session details – like date, time, duration, and service type – because there’s no auto-sync feature. To make matters worse, therapy notes and medication management systems often exist in separate silos, requiring even more manual data entry.
The toll of these inefficiencies is undeniable. Nearly 75% of providers who report burnout cite their EHR as a major contributor. On top of that, constant task-switching – estimated at 1.4 times per minute – breaks concentration and wastes over an hour of productivity every day. For a clinic with 10 clinicians, this can translate to financial losses exceeding $120,000 annually. Beyond the financial impact, these inefficiencies disrupt workflows and can ultimately compromise the quality of care.
“In today’s Behavioral health landscape, administrative demands can diminish both provider efficiency and client care. The number one complaint was that typing notes took too much time.”
– Tabatha Golding, Senior Vice President of Operations, Beacon Outpatient Management
Some organizations are already finding ways to tackle this issue. Take GRAND Mental Health in Oklahoma as an example. In January 2024, they introduced an AI-driven system to automate progress notes. Just six months later, the system was completing more than 80% of each note, saving over 400 staff hours and cutting documentation time by more than half.
This kind of innovation shows what’s possible when technology is designed to truly meet the needs of clinicians. It’s a step toward reducing the administrative burden and giving clinicians more time to focus on what matters most – their patients.
You Lack Visibility Across Programs
Trying to manage residential and outpatient programs without clear, actionable data makes decision-making a guessing game. Leadership teams need immediate answers to critical questions like: Are residential beds at capacity? Are clinicians meeting their performance goals? Where are intake delays slowing down admissions? Is incomplete documentation holding up billing? If your EHR system can’t provide these answers quickly, you’re left making decisions in the dark.
The challenge becomes even greater when residential and outpatient programs operate on separate systems. Patient data gets scattered across silos, making it almost impossible to access essential information – like care plans or medication lists – when patients move between levels of care. Staff are often forced to manually piece together data, a time-consuming and error-prone process that delays responses to urgent issues. In fact, 69% of healthcare providers report major interoperability challenges between their EHR and other systems.
“If your current EHR can’t easily track important metrics across your practice, you’re working blind.”
The lack of integrated analytics doesn’t just hinder day-to-day operations – it can also cost you in the long run. For instance, without robust reporting, it’s hard to pinpoint which programs are profitable or identify the best payer reimbursement strategies. Worse, inadequate reporting could prevent your facility from achieving key certifications like JCAHO or CARF, which demand detailed, comprehensive process documentation.
For organizations managing multiple locations and services, relying on manual data aggregation can take days instead of minutes. By the time the reports are ready, the situation on the ground has likely changed. Behavioral health organizations need systems that provide instant, real-time visibility across the entire care continuum. Outdated, disconnected systems don’t just slow you down – they also limit your ability to grow and adapt effectively.
Your System Doesn’t Scale as Your Organization Grows
As organizations grow, scaling their operations should become smoother – not more complicated. Unfortunately, if your EHR system wasn’t built to handle multiple levels of care, every new program, location, or service line adds unnecessary complexity instead of simplifying workflows. What starts as a manageable system can quickly spiral into chaos when stretched across residential, outpatient, and intensive outpatient (IOP) services.
Many organizations end up stuck with “single-serve” platforms that require separate software for each program. For instance, you might use one system for residential care and another for outpatient services. This leads to fragmented data, duplicated efforts, and disconnected workflows. Staff are forced to waste time switching between systems, and critical patient details often get lost during transitions between care levels. Instead of fostering efficiency, this disjointed setup drains productivity and creates more barriers.
To bridge the gaps, organizations often turn to third-party tools for scheduling, billing, or communication. But each new tool adds its own set of challenges – another login, another training session, and more time spent navigating between platforms. What’s worse, the added tools can actually increase inefficiency. Research shows that clinicians working with disconnected systems face an average of 1.4 task switches per minute, resulting in over an hour of lost productivity every day.
“The most impactful elements for us are being able to manage so many different types of services that we offer and being able to customize the software to meet the programs we are implementing.”
– Katharine Spehar, Director of HR and Operations, Southwest Family Guidance Center
Scalability issues are particularly glaring during mergers and acquisitions. When your EHR system is inflexible, integrating data from a newly acquired practice becomes a monumental task, often requiring months of manual effort to consolidate patient records. If your technology can’t keep up with your growth strategy, it’s not just an operational headache – it’s a roadblock to expanding services and meeting the increasing demand for behavioral health care.
Staff Are FrustratedWiththe System
When an EHR system doesn’t align with behavioral health workflows, frustration among staff quickly escalates. Inefficient systems force employees to rely on makeshift solutions – like spreadsheets or paper backups – to manage information that should ideally be handled within the EHR itself.
These daily hurdles take a toll on both efficiency and morale. In fact, 60% of behavioral health professionals cite EHR frustrations as a key factor in burnout. Common complaints include navigating through endless screens, struggling to locate patient details spread across disconnected platforms, and repeatedly entering the same data. For example, clinicians often find themselves retyping basic appointment details into separate notes, a process that’s both time-consuming and draining. This constant inefficiency wears down morale and creates ripple effects across the organization.
“In healthcare, redundancy accounts for one of the biggest wastes in terms of resource allocation.” – Dylan Souza, Vice President of Marketing, ContinuumCloud
These inefficiencies don’t just affect individual productivity – they also create organizational challenges. Staff members frequently stay late to complete documentation or scramble to find vital information during patient transitions. Over time, this leads to decreased job satisfaction and higher turnover rates.
The problem extends beyond morale. When employees spend more time wrestling with outdated systems than focusing on patient care, expanding services becomes a challenge. New hires require longer training periods to navigate unintuitive software, while seasoned clinicians may leave for workplaces with better tools. Purpose-built EHR software, however, can cut documentation time by 30% to 50%, allowing staff to dedicate more energy to providing quality care. Addressing these frustrations is critical to creating systems that genuinely support behavioral health teams.
Comparison Table
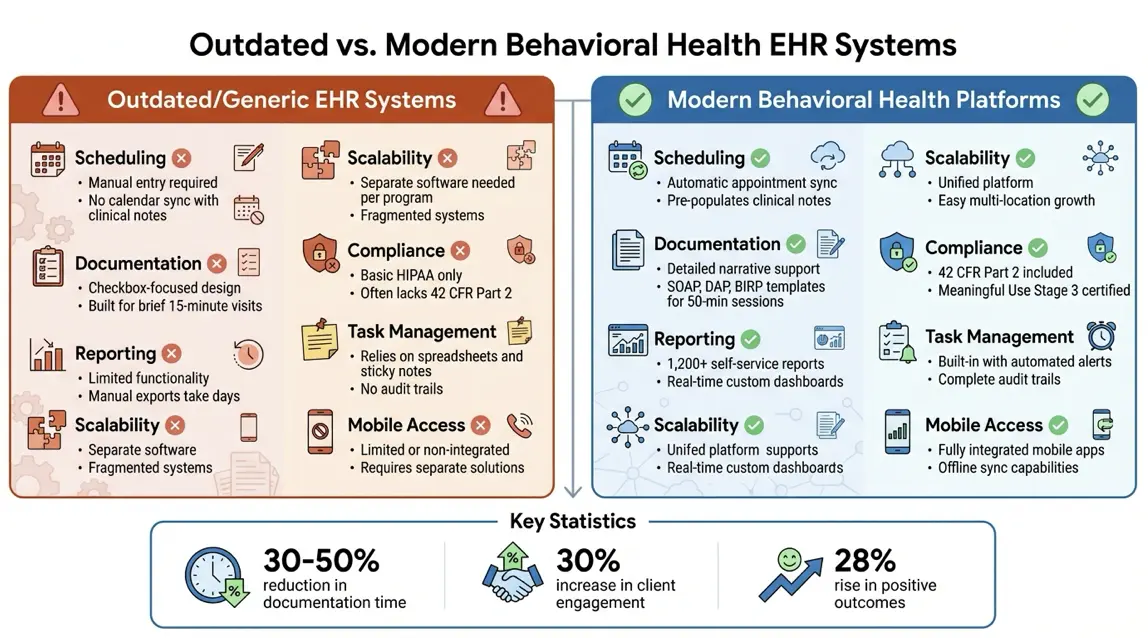
Here’s a side-by-side look at how outdated or generic EHR systems stack up against modern behavioral health platforms:
| Feature | Outdated/Generic EHR Systems | Modern Behavioral Health Platforms |
| Scheduling | Requires manual entry; calendar data doesn’t sync with clinical notes. | Automatically syncs appointments, pre-populating clinical notes. |
| Documentation | Focused on checkboxes, suited for brief visits. | Supports detailed narratives with SOAP, DAP, and BIRP templates for longer sessions. |
| Reporting | Limited functionality; manual exports take days to compile data. | Offers over 1,200 self-service reports and real-time custom dashboards. |
| Scalability | Needs separate software for different programs. | Unified platform that easily supports multi-location growth. |
| Compliance | Basic HIPAA compliance; often lacks 42 CFR Part 2 segmentation. | Includes 42 CFR Part 2 and Meaningful Use Stage 3 certifications. |
| Task Management | Relies on external tools like spreadsheets or sticky notes. | Built-in task management with automated alerts and audit trails. |
| Mobile Access | Limited or requires separate, non-integrated solutions. | Fully integrated mobile apps (e.g., Welligent Express) with offline sync capabilities. |
These modern features enable smoother operations, allowing staff to focus on what matters most: patient care.
“We have numerous programs, and we can adapt the configuration based on program needs and documents. I think that’s been very advantageous for us.” – Glenda Pittman, Finance and IS Division Director, Arlington County Community Services Board
When your system auto-populates documentation, generates reports in real time, and operates as one cohesive unit, your team can dedicate their energy to providing exceptional care. Aligning your technology with the specific needs of behavioral health ensures seamless support across all programs.
Conclusion
Outdated EHR systems create challenges at every level of care in behavioral health. When these systems force residential staff to juggle spreadsheets, overwhelm clinicians with excessive documentation, or leave leadership in the dark without clear insights, the result is lost productivity, higher costs, and dissatisfied staff.
Inefficiencies in documentation alone can cost a clinic significantly. For example, clinicians lose up to 20 minutes each day due to outdated systems – translating to over $120,000 annually for a 10-clinician clinic. Additionally, 60% of behavioral health professionals cite EHR frustrations as a major factor in burnout. These aren’t just inconveniences; they are obstacles that hinder your ability to deliver quality care.
Switching to a unified, purpose-built platform can make a huge difference. By streamlining workflows and eliminating redundant data entry, such systems improve care coordination. When residential and outpatient programs operate seamlessly within the same platform, your team can shift focus from workarounds to what truly matters – your clients. In fact, organizations using specialized behavioral health software report a 30% increase in client engagement and a 28% rise in positive outcomes.
“With Welligent it’s right there, we train our staff to use it, we train our staff to reference it, there are no drops of information that are really essential to our clients.” – Jeremy Ulderich, Senior Reporting Analyst, Grafton Integrated Health Network




