Disconnected systems in healthcare create inefficiencies that waste time, drain resources, and harm both patient care and staff satisfaction. Here’s the bottom line:
- Time Waste: Staff spend 10–20+ hours weekly on redundant tasks like manual data entry and troubleshooting.
- Financial Losses: Inefficiencies cost U.S. healthcare $90–$140 billion annually, with claim denial rates as high as 10%.
- Burnout Crisis: 78% of behavioral health clinicians report burnout, with 40% of positions unfilled due to administrative overload.
- Patient Impact: Scattered data delays care, worsens outcomes, and erodes trust.
Unified systems, like those offered by ContinuumCloud, address these challenges by integrating clinical, workforce, and engagement tools. This reduces manual work, lowers costs, and improves care delivery. For example, organizations using integrated platforms report 30% less administrative time, 25-35% better patient adherence, and significant reductions in staff burnout.
Disconnected systems aren’t just an inconvenience – they’re a costly barrier to better healthcare.
How Siloed Systems Disrupt Daily Operations
When clinical, workforce, and engagement platforms fail to communicate, staff are left to fill in the gaps manually. These disconnected systems create friction at every step – whether it’s front-desk intake, clinical documentation, or billing. Instead of supporting operations, technology becomes another hurdle, leading to delays and inefficiencies like those outlined below.
Manual Data Entry and Workflow Delays
Disconnected platforms mean staff must repeatedly re-enter the same information across multiple systems. For instance, a patient’s medication list entered during intake doesn’t automatically populate in the clinical notes. Scheduling adjustments in one system must be manually updated in another, and billing requires prescription details to be retyped yet again.
This redundancy wastes time and resources. UnityPoint Health faced this issue before adopting the Corepoint Integration Engine in 2026. By modernizing their systems, they achieved over 1,000 days without unplanned downtime, cutting maintenance costs and reducing the need for manual IT interventions.
Data Gaps and Fragmented Information
Beyond redundant tasks, disconnected systems create critical data gaps that disrupt care. Key information – like intake responses or post-visit updates – often fails to sync with the central chart. This forces providers to repeatedly ask patients the same questions, which not only wastes time but also erodes trust. Patients notice when they’re asked to recount their history at every visit, and this can lead to frustration and disengagement from treatment.
Transitions in care are another weak point. When a patient moves from residential to outpatient treatment, medication lists and treatment histories don’t always transfer seamlessly. Staff are left scrambling to track down these details, while leadership struggles with incomplete performance metrics.
Missed Opportunities in Patient Care
Operational delays caused by fragmented systems can directly impact clinical care, delaying treatment and worsening outcomes. Scattered data prevents real-time insights, which are often crucial in mental health care. On average, patients with severe mental illness face delays of 8 to 10 years from symptom onset to receiving proper treatment. Disconnected systems only make these delays worse, increasing the likelihood of severe episodes and hospitalizations. Patients with serious mental illness are 2.5 times more likely to visit the emergency room than the general population.
“Fragmentation doesn’t save money, but it changes who suffers. It could be the patient, the clinician, the staff member, or the healthcare system.”
- Azizi A. Seixas, PhD, Associate Professor, University of Miami Miller School of Medicine
Cleveland Clinic tackled these issues in March 2026 by implementing prior-authorization automation. This system notified providers of authorizations 6 to 7 days faster and completed peer-to-peer review adjudications 11 days sooner, helping to reduce treatment delays for patients.
“When systems don’t talk to each other, staff become the integration.”
- Mia Ballan, LifeLoop
Each handoff in a fragmented system adds what amounts to a “hidden tax”, creating administrative waste and forcing staff to bridge the gaps manually. This inefficiency puts unnecessary strain on both staff and the patients who rely on timely, coordinated care.
Financial Costs: Measuring the Impact of Inefficiencies
Disconnected systems in healthcare create operational challenges that translate into real financial losses. In the U.S., about 25% of healthcare spending goes toward administrative tasks, with inefficiencies costing between $90 billion and $140 billion annually. For behavioral health organizations, which often operate on tight margins, these inefficiencies can be the deciding factor between staying afloat or shutting down. The financial burden begins with administrative processes.
Increased Administrative Costs
When systems don’t communicate, staff are left to manually fill the gaps, leading to duplicated efforts. For instance, medical office staff spend 15–20 hours each week managing phone calls for scheduling and reminders. On top of that, they dedicate 5–8 hours to duplicate data entry, 4–6 hours to insurance verification and prior authorization, and 3–5 hours each to billing follow-ups and scheduling changes. Altogether, this adds up to a staggering 30–44 hours of wasted administrative time per week for a single practice.
“The average physician in the U.S. now spends close to two hours on administrative work for every hour of direct patient care.”
- Aubreigh Lee Daculug
This workload doesn’t end when the office closes. Clinicians often spend 1.4 hours after hours completing tasks in electronic health records (EHRs) that could have been streamlined during the day. This eats into personal time and contributes to burnout. Meanwhile, the constant switching between unconnected applications disrupts focus, costing over an hour of productivity per staff member every day.
Revenue Loss from Missed Billing
Administrative inefficiencies don’t just waste time – they also threaten revenue. Disconnected systems create data gaps that lead to claim denials and delayed reimbursements. In fact, 79% of behavioral health organizations report increased claim denials due to these gaps. Denial rates often range between 5–10% of all claims, and many practices simply write off denied claims because the cost of investigating and resubmitting them outweighs the potential reimbursement.
Slow billing processes and claim rework can delay revenue by 30–60 days, creating cash flow problems. No-shows add another layer of loss, typically costing $150 to $300 per missed appointment. Just five no-shows per week can lead to over $50,000 in lost revenue annually. However, integrated EHR systems can significantly reduce these losses. For example, practices using integrated EHRs report claim denial rates of less than 1% and see 26% lower per-member-per-month costs.
Higher Turnover and Recruitment Expenses
The financial impact of inefficiencies doesn’t stop at revenue – it also drives up staffing costs. Administrative overload not only drains budgets but also contributes to employee burnout. Replacing a single employee can cost between $30,000 and $50,000. Losing just two employees annually due to burnout can result in $60,000 to $100,000 in replacement costs. With 78% of behavioral health providers experiencing burnout and 40% of positions remaining unfilled, the remaining staff often take on extra work, which accelerates turnover.
“Research consistently links administrative overload to physician burnout – and burnout creates its own set of costly ripple effects, from increased errors to higher physician turnover rates that are far more expensive to address than the underlying administrative problems.”
- Aubreigh Lee Daculug
Modern clinicians now expect access to tools that save time and reduce stress. For example, in May 2024, Coleman Health Services adopted an AI-powered documentation platform integrated with their Welligent EHR. This reduced documentation time by 70% and improved note submission timeliness from five days to just 1.5 days, achieving a 92% satisfaction rate among clinical staff. These examples underline the importance of unified systems in addressing inefficiencies and reducing costs in behavioral health.
Human Impact: Burnout and Workforce Challenges
Disconnected systems don’t just drain finances – they take a heavy toll on the people working in behavioral health. These inefficiencies don’t just inflate costs or slow down care; they also harm clinician satisfaction and retention. For those on the front lines, dealing with clunky systems adds extra stress to an already demanding job. Behind the statistics are real individuals trying to provide quality care while battling outdated or inefficient technology.
Administrative Burden and Burnout
When systems don’t communicate, clinicians are left manually re-entering data and transferring information across platforms. What should be smooth workflows become time-consuming hurdles. The numbers paint a stark picture: 78% of behavioral health clinicians experience burnout, while staff vacancy rates exceed 40%. Instead of focusing on patient care, providers spend between 34% and 55% of their day on documentation. On average, manual note-taking eats up 10–12 minutes per session, but AI-powered systems can cut this down to under 3 minutes.
“With clinicians stressed and overburdened, patients simply aren’t going to receive the best care possible.”
- Dror Zaide, Co-founder and COO, Eleos Health
The problem doesn’t stop when the workday ends. Clinicians spend about 1.4 hours after hours completing EHR tasks, which erodes their personal recovery time and speeds up burnout. A Yale New Haven Health study involving 272 clinicians between February and October 2024 showed promising results: ambient AI scribes reduced burnout rates from 52% to 39% in just 30 days, while cutting after-hours documentation by nearly one hour per week.
Cognitive Overload and Reduced Job Satisfaction
The stress isn’t just about the volume of work – it’s also about the constant mental juggling. Clinicians switch tasks an average of 1.4 times per minute, disrupting their focus and shaving over an hour off their daily productivity. This relentless task-switching leads to cognitive overload, which lowers job satisfaction and reduces clinical effectiveness. Burned-out clinicians report a client improvement rate of only 28.3%, compared to 36.8% for those who aren’t burned out. When clinicians are distracted by multiple systems, they can’t fully concentrate on their patients, and the quality of care inevitably suffers.
“The fact that you can have an encounter with a patient and focus on that patient with all the cognitive skills that are required of us… it’s liberating.”
- Dr. Leopoldo Pozuelo, Center Director of Adult Behavioral Health, Cleveland Clinic
This ongoing pressure doesn’t just harm performance – it pushes many clinicians to leave their roles altogether.
Impact on Employee Retention
Disconnected systems are now a major factor in employee retention. Clinicians increasingly see access to efficient, integrated technology as a must-have when choosing where to work. In a tight labor market where behavioral health organizations struggle to fill positions, outdated or cumbersome systems become a dealbreaker. By adopting unified systems that ease the administrative load, organizations can create environments where clinicians feel supported – and are more likely to stay.
Solutions: How Unified Systems with ContinuumCloud Address These Challenges

Disconnected systems don’t have to be the norm. ContinuumCloud tackles these inefficiencies directly, simplifying processes and addressing the operational and financial hurdles discussed earlier. By uniting clinical, workforce, and engagement functions into a single ecosystem, ContinuumCloud eliminates the need for staff to juggle multiple platforms. This seamless data flow not only cuts down on silos but also reduces the friction that contributes to burnout and inefficiency.
Integration of Welligent, DATIS, and CaredFor

ContinuumCloud brings together three key platforms: Welligent for electronic health records and clinical documentation, DATIS for workforce scheduling and compliance, and CaredFor for patient engagement through secure messaging and personalized resources. These systems are designed to communicate in real time.
For example, when a clinician updates a patient’s treatment progress in Welligent, that information syncs instantly with DATIS to adjust staff schedules and with CaredFor to send automated patient reminders. One behavioral health clinic saw a 40% drop in scheduling errors and improved appointment adherence thanks to this real-time integration. The “Golden Thread” functionality ensures that assessments, treatment plans, and progress notes remain aligned, meeting regulatory standards while reducing manual reconciliation.
The system also includes automated position control, ensuring that only properly licensed and trained staff are scheduled for specific roles. Field-based staff can document care even without Wi-Fi, with data syncing automatically once connectivity is restored. This integration creates smoother workflows and sets the stage for significant time savings.
Streamlined Workflows and Improved Efficiency
Unified systems remove the need for redundant data entry, saving valuable staff time. Organizations using ContinuumCloud report 30% less administrative time and 20-40% fewer hours spent on manual tasks. For instance, Welligent’s AI-powered documentation tools cut note-taking time from 10-12 minutes per session to under 3 minutes. These time savings allow clinicians to spend more time with patients and less time on after-hours work.
“Together we’re giving clinicians their time back while ensuring defensible, compliant documentation.”
- Bob Bates, CEO, ContinuumCloud
DATIS leverages clinical data from Welligent to optimize staffing, matching staff skills with patient needs through shared dashboards and automated alerts. Real-time visibility into bed availability and staffing capacity also prevents overbooking. After integration, organizations reported an increase in on-time task completion from 65% to 92%.
Better Engagement and Care Outcomes
These unified systems don’t just lighten staff workloads – they also enhance the patient experience. CaredFor’s tools, such as secure messaging, educational resources, progress tracking, and automated SMS reminders, pull data directly from Welligent and sync with DATIS for staff notifications. This ensures patients receive timely, tailored support that reflects their treatment status while maintaining HIPAA compliance.
The results speak for themselves: syncing engagement tools with clinical records boosts patient adherence by 25-35%. Providers using these systems have also seen a 35% increase in the use of evidence-based techniques during sessions. For instance, GRAND Mental Health implemented ContinuumCloud’s AI system in January 2024, which automated over 80% of progress notes and saved more than 400 staff hours in six months. Another behavioral health provider reported a 28% reduction in staff burnout, as clinicians gained 10-15 hours of time back each week from reduced administrative tasks.
When clinicians focus less on paperwork and more on direct care, patients benefit. Personalized, timely communication keeps patients engaged, while staff supported by efficient technology are more likely to stay motivated and committed.
Measurable Results: Disconnected vs. Unified Systems
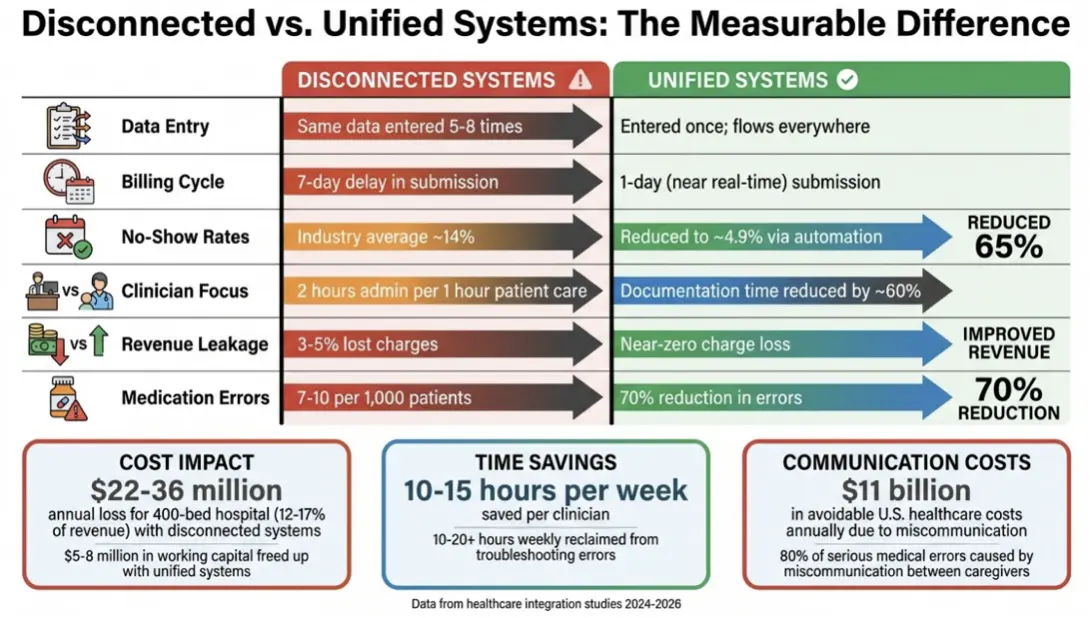
The hidden costs of fragmented systems become glaringly obvious when you compare measurable results. Unified systems consistently deliver better outcomes in terms of cost savings, time efficiency, error reduction, and scalability. Organizations that switch to a unified approach see improvements across operations, reduced errors, and smoother growth without unnecessary complications.
Cost and Time Savings
The financial burden of disconnected systems is staggering. Take a 400-bed hospital generating $300 million annually – these inefficiencies cost $22–$36 million per year, or about 12% to 17% of total revenue, lost to administrative waste.
Unified systems address this by eliminating repetitive data entry, where the same information is often entered 5–8 times. Instead, data flows automatically from its initial input to all relevant departments. This cuts billing delays from 7 days to just 1 day. For mid-sized hospitals, such efficiency can free up $5–$8 million in working capital by reducing Days Sales Outstanding by about 15 days.
One medical practice saw its no-show rate drop from 14.20% to 4.91% within three months by using telehealth and appointment reminders. This improvement translated into a 10% to 20% boost in recovered revenue by filling previously empty appointment slots. Additionally, clinicians save 10–15 hours per week by eliminating redundant documentation and manual tasks, which also reduces error risks.
|
Metric |
Disconnected Systems |
Unified Systems |
|
Data Entry |
Same data entered 5–8 times |
Entered once; flows everywhere |
|
Billing Cycle |
7-day delay in submission |
1-day (near real-time) submission |
|
No-Show Rates |
Industry average ~14% |
Reduced to ~4.9% via automation |
|
Clinician Focus |
2 hours admin per 1 hour care |
Documentation time reduced by ~60% |
|
Revenue Leakage |
3–5% lost charges |
Near-zero charge loss |
Error Reduction and Improved Accuracy
Fragmented systems open the door to errors at nearly every step. Manual data transfers often lead to mistakes, such as incorrect dosages or missed allergy alerts. In such environments, medication errors occur at a rate of 7 to 10 per 1,000 patients. Unified systems, on the other hand, prevent up to 70% of these errors by using automated cross-checks that flag issues like drug interactions or unsafe dosages in real time.
“80% of serious medical errors are caused by miscommunication between caregivers.” – HIPAA Journal
Poor communication and data gaps contribute to over $11 billion in avoidable healthcare costs annually in the U.S.. Unified platforms address these issues, with some teams reclaiming 10 to 20+ hours weekly that were previously wasted on troubleshooting data errors.
Disconnected systems also lead to 3% to 5% of charges being lost due to missed documentation or coding errors. Unified platforms automate charge capture directly from clinical activities, minimizing losses and enabling cleaner claims, faster reimbursements, and fewer denied payments. This increased accuracy not only saves money but also lays a solid foundation for scaling operations.
Scalability and Growth
Unified systems simplify growth by providing a stable infrastructure that doesn’t buckle under expansion. For instance, West Virginia University Health System used the Rhapsody platform to centralize its integration strategy during a period of rapid mergers. This reduced interface development time by over 50%, allowing new hospitals to be onboarded quickly.
Similarly, UnityPoint Health transitioned from fragmented interfaces to the Corepoint Integration Engine, achieving over 1,000 days without unplanned downtime. This move significantly cut maintenance costs while enhancing reliability. Such operational stability is critical when scaling, as it ensures smooth integration of new locations without disrupting ongoing operations.
Unified platforms also make it easier to adopt new technologies and meet regulatory standards. Instead of building custom integrations for every vendor or compliance requirement, teams can use modular architectures that adapt quickly. This flexibility prevents stagnation and keeps organizations competitive in a constantly evolving healthcare landscape.
The financial upside is undeniable. Fragmentation can drain hospitals of 12% to 17% of their annual revenue. By eliminating these inefficiencies, unified systems enable organizations to grow – serving more patients, expanding services, and achieving better outcomes without the usual administrative headaches. These measurable results highlight the transformative potential of a unified approach.
Conclusion: The Benefits of Integration
Disconnected systems might not seem like a big deal at first, but over time, they quietly drain resources and create inefficiencies that ripple across every department. Manual data entry, billing delays, and fragmented information lead to operational headaches that no organization can afford to ignore.
Integration changes everything. With a smooth flow of data, redundant tasks and manual workarounds disappear, allowing clinicians to focus on what they do best – caring for patients. On the financial side, fewer administrative delays mean faster billing and less revenue slipping through the cracks. Plus, staff no longer have to juggle multiple platforms, reducing the fatigue and frustration that often lead to burnout.
These improvements create a foundation for a more streamlined and effective organization. ContinuumCloud’s integrated approach – bringing together Welligent, DATIS, and CaredFor – provides a single, reliable source of truth. This isn’t just about convenience; it addresses the staggering $11 billion lost annually due to data gaps and miscommunication. When residential programs, workforce scheduling, and engagement tools work in harmony, the entire system becomes more efficient.
The result? Greater operational efficiency, better patient care, and a more empowered workforce. Organizations face a choice: continue to absorb the costs of disconnected systems or embrace a unified platform to eliminate them. By choosing integration, they set the stage for sustainable growth, improved outcomes, and a team that can focus on what truly matters.
FAQs
What are the biggest hidden costs of disconnected healthcare systems?
These inefficiencies also create financial challenges. Higher operational expenses, delayed billing processes, and potential compliance risks can all weigh heavily on an organization’s budget. But the impact doesn’t stop there – outdated systems can directly affect patient safety. Errors such as missed drug interactions or delays in care can not only harm patients but also lead to expensive legal settlements and other preventable consequences.




