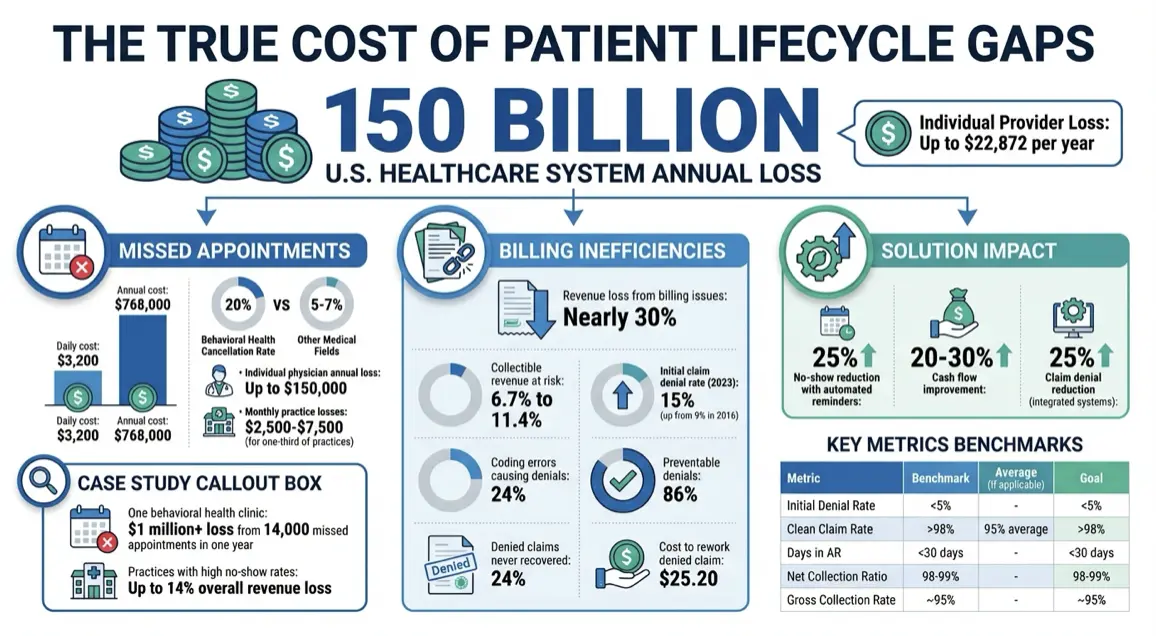
Missed appointments, treatment drop-offs, and delayed payments are draining healthcare providers’ revenue – costing the U.S. healthcare system $150 billion annually. For individual providers, this can mean losses of up to $22,872 per year. Beyond the financial hit, these gaps disrupt operations, create inefficiencies, and harm patient outcomes, especially in fields like behavioral health, where ongoing engagement is critical.
Key takeaways:
- Missed appointments can cost practices $3,200 daily or $768,000 annually.
- Billing inefficiencies like undercoding and claim denials account for nearly 30% of revenue loss.
- Behavioral health faces unique challenges, with 20% cancellation rates and complex billing requirements.
The solution? Integrated patient lifecycle management. Tools like automated reminders, real-time eligibility checks, and streamlined billing systems can reduce no-shows by 25%, improve cash flow by 20-30%, and recover lost revenue. Focus on metrics like denial rates, clean claim rates, and days in accounts receivable to identify and address revenue leaks.
The Cost of Disengagement: How Lifecycle Gaps Drain Revenue
Calculating Revenue Losses
Lifecycle gaps can jeopardize 6.7% to 11.4% of collectible revenue, primarily due to patient disengagement. For behavioral health providers, the stakes are even higher, as mental health settings often experience a 20% cancellation rate – nearly triple the 5–7% average seen in other medical fields.
Here’s a stark example: a practice with an average revenue of $160 per visit and 20 daily no-shows loses $3,200 every day. Over a year, that adds up to $768,000. For individual physicians, missed appointments can result in personal revenue losses of up to $150,000 annually. Additionally, more than one-third of practices report losing between $2,500 and $7,500 monthly due to cancellations and no-shows. These figures highlight the financial toll lifecycle gaps can take, as illustrated in the following case study.
Case Study: A Clinic’s Revenue Loss from Lifecycle Gaps
One behavioral health clinic faced over $1 million in losses in a single year due to 14,000 missed appointments. The impact wasn’t just financial – empty slots disrupted schedules, staff spent countless hours rescheduling patients, and entire treatment plans fell apart when patients disengaged after multiple no-shows.
According to a 2021 MGMA report, practices with high no-show rates could lose up to 14% of their overall revenuebecause of missed appointments and delayed payments. This clinic’s experience echoed that finding. Lifecycle inefficiencies left significant amounts of revenue unposted and unnoticed until a comprehensive audit revealed the full extent of the problem.
Hidden Losses Beyond Denials
The financial drain doesn’t stop at no-shows. Administrative issues, like undercoding and billing delays, further chip away at revenue. Undercoding happens when providers fail to document services thoroughly, leaving potential earnings unclaimed, even for completed appointments. Timeliness decay occurs when reimbursement rates drop because claims aren’t submitted quickly enough. And unbilled services accumulate when documentation gaps prevent billing altogether.
When 27% of healthcare professionals attribute revenue losses to appointment disruptions, many are only scratching the surface. These billing inefficiencies add another layer to the financial challenges practices face, underscoring the pressing need for better lifecycle management strategies.
Why Lifecycle Gaps Happen in Behavioral Health
Revenue Cycle Challenges in Behavioral Health
Behavioral health providers face a unique set of hurdles when it comes to billing. Unlike general practices, they deal with session-based billing, which demands precise documentation for every encounter – whether it’s an individual therapy session, group counseling, or family therapy. Each service requires specific codes, leaving little room for mistakes. Adding to the complexity, payer policies and coverage requirements frequently change. A coding method that worked smoothly last month might suddenly result in claim denials today. By 2023, about 15% of initial claims were denied – up significantly from 9% in 2016 – showing just how challenging the landscape has become. These issues directly lead to revenue losses, as gaps in documentation and coding prevent practices from collecting the payments they’ve earned.
“A well-optimized revenue cycle lets you predict timely reimbursements and a healthy cash flow.”
– Sunwave Health
Another major issue is the disconnect between clinical care and billing and revenue cycle management. Therapists naturally prioritize patient care over making sure their notes meet the intricate standards required for reimbursement. This misalignment means revenue is lost, even when care is delivered flawlessly. The problem worsens when clinical and billing systems fail to integrate, creating inefficiencies and errors.
How Disconnected Systems Create Gaps
Many behavioral health practices rely on separate systems for scheduling, clinical documentation, and billing. For example, a patient might book an appointment in one platform, their session gets recorded in another, and billing happens in yet another system. These handoffs increase the likelihood of errors – like missing fields or transcription mistakes. In November 2025, Sunwave Health emphasized that disconnected systems are a major source of claim denials and revenue leakage for behavioral health organizations.
One clinic that adopted an integrated EHR and billing system in August 2025 saw a 25% drop in claim denials within just six months. Their cash flow improved by 30%, thanks to streamlined processes like automated eligibility checks and eliminating the need for duplicate data entry.
Common Denial Causes and Process Failures
Authorization issues are the top reason for claim denials. When services are provided without pre-authorization or with incorrect authorizations, practices can lose thousands of dollars every month.
“Authorization missing or invalid remains one of the most common denial categories across hospitals, clinics, and specialty providers.”
– RCA Team
Coding errors account for 24% of claim denials. Even small mistakes, like billing for a 45-minute session (90834) instead of a 60-minute session (90837), can lead to automatic rejections. Documentation gaps add another layer of complexity – if therapists don’t clearly demonstrate the medical necessity of a service, payers may deny the claim outright. These types of errors directly contribute to the revenue losses discussed earlier, as they prevent practices from being reimbursed for services they’ve already provided.
“Providers lose revenue because appeal windows close before staff reach the claim.”
– RCA Team
Registration mistakes, such as a misspelled name, incorrect date of birth, or outdated insurance details, can derail claims before they even get processed. Nearly 30% of revenue is lost due to these types of inefficiencies. These challenges highlight the importance of integrated lifecycle management solutions, which will be explored in the next section.
How Integrated Lifecycle Management Closes the Gaps
The financial losses highlighted earlier demand a proactive approach, and integrated lifecycle management steps in to provide practical solutions that address these challenges head-on.
Preventing Front-End Revenue Losses
Stopping revenue leakage starts with catching issues early. Automated eligibility checks confirm insurance coverage as soon as a patient schedules an appointment, ensuring payments are accurate from the outset. Additionally, tracking pre-authorizations ensures all necessary approvals are in place before services are delivered, significantly reducing the risk of claim denials later.
Automated appointment reminders play a critical role in reducing no-shows – by as much as 25% according to some studies. For example, in 2025, a practice using integrated eligibility verification and reminders saw missed appointments drop by 30%, leading to a 20% boost in cash flow. Considering that no-shows cost practices an average of $22,872 annually, these systems quickly pay for themselves.
“Automated appointment reminders have been proven to lower no-show rates by up to 25%. This reduction helps providers retain planned appointment revenue.”
– CompuGroup Medical
With front-end losses under control, the next focus turns to improving documentation accuracy.
Improving Documentation and Coding Accuracy
Integrated systems reduce errors by streamlining the flow of clinical documentation into billing processes. This eliminates many manual handoffs, which are often the source of mistakes. By automating data transfer and removing duplicate entries, these systems ensure billing codes are applied correctly and consistently. The result? Fewer documentation errors, faster reimbursements, and more time for clinicians to focus on patient care instead of administrative tasks.
Automating Payment Posting and Revenue Tracking
Manual payment posting can be riddled with errors, but automated systems solve this by reconciling payments as they come in. These systems match payments to the correct patient accounts and flag discrepancies in real time. Real-time dashboards further enhance transparency by showing pending claims, received payments, and follow-up actions.
“Using AI to enable the revenue cycle could lead to a 30 to 60 percent reduction in cost to collect, faster cash realization, and a workforce refocused on patient value rather than administrative tasks.”
– McKinsey
This automation not only reduces administrative burdens but also allows staff to focus on more complex tasks, like resolving denied claims and improving patient experiences. With nearly 20% of claims denied on average – and up to 60% of those denials going unchallenged – automated tracking ensures no revenue opportunity is overlooked. These tools not only protect immediate cash flow but also lay the groundwork for stronger, long-term revenue management.
Key Metrics for Tracking Revenue Recovery
Measuring the right metrics turns vague revenue concerns into clear, actionable steps. These numbers help convert streamlined processes into measurable gains, pinpointing where revenue leaks occur and guiding efforts to fix them.
Monitoring Denial Rates and Billing Efficiency
Denial rates are a direct indicator of revenue leakage. Ideally, this rate should stay below 5%. Alarmingly, while 86% of denials are preventable, 24% of denied claims are never recovered, leading to permanent revenue loss. On average, reworking a denied claim costs $25.20.
Another critical metric is the Clean Claim Rate (CCR) – the percentage of claims accepted on their first submission. High-performing practices aim for a CCR of at least 98%, compared to the industry average of 95%. A low CCR often signals issues like insufficient staff training or outdated electronic medical record systems, both of which can disrupt billing accuracy.
Days in Accounts Receivable (DAR) is another key measure, showing where cash flow bottlenecks occur. For physician practices, DAR should stay under 30 days. For example, in 2025, a behavioral health clinic reduced its DAR from 45 to 25 days by adopting a new revenue cycle management system. This system included real-time eligibility verification and automated billing. Under the leadership of billing manager John Smith, the clinic saw a 30% boost in cash flow within six months (Source: SimiTree, 2025).
|
KPI |
Industry Benchmark |
What It Reveals |
|
Initial Denial Rate |
< 5% |
Revenue leakage and administrative inefficiency |
|
Clean Claim Rate |
> 98% |
Billing accuracy and workflow effectiveness |
|
Days in AR |
< 30 Days |
Cash flow efficiency and collection speed |
|
Net Collection Ratio |
98% – 99% |
Overall revenue capture effectiveness |
These metrics provide a solid foundation for evaluating broader trends, including patient engagement and retention.
Tracking Patient Engagement and Retention
Patient engagement metrics reveal how effectively your practice manages the patient lifecycle. Missed appointments are more than scheduling hiccups – they represent lost revenue. Practices that use personalized appointment reminders and telehealth options have reduced no-show rates by up to 25%.
“Engaged patients are more likely to keep appointments.”
– Cadence Collaborative
Attendance and contact rates are also key indicators of how well patients interact with your practice regarding outstanding balances or scheduling. On average, more than a third of practices lose up to $7,500 monthly due to cancellations and no-shows. Offering same-day appointments and telehealth options – now available at 69% of practices – has proven effective. In fact, 71% of patients say same-day availability makes them less likely to cancel.
Beyond engagement, tracking revenue per patient encounter gives an even clearer picture of financial performance.
Revenue Per Patient Encounter
Revenue per patient encounter – calculated as total collections divided by total visits – can highlight billing issues that denial rates might miss. For example, if your denial rate looks fine but revenue per encounter is dropping, you might be dealing with undercoding or missed billing opportunities. This metric offers a direct link between improved processes and better revenue capture.
Healthcare settings lose nearly 30% of revenue due to inefficient billing practices. However, practices that invest in comprehensive revenue cycle management technology often see a 20–30% improvement in cash flow within the first year. Monitoring revenue per encounter ensures you’re capturing the full value of each visit and not losing money to incomplete documentation or overly cautious coding.
“What gets measured, gets managed.”
– Experian Health
Another useful metric is the Gross Collection Rate (GCR) – the percentage of total patient balances actually collected. A strong GCR should hover around 95%. When paired with revenue per encounter data, this metric helps identify whether low collections are due to billing errors, patient payment challenges, or systematic undercoding. Addressing these issues often requires better clinical documentation and coding practices.
Conclusion: Converting Lifecycle Gaps Into Revenue Gains
Patient lifecycle gaps aren’t just frustrating – they’re a direct hit to revenue, causing avoidable losses across the healthcare industry. But here’s the good news: these gaps aren’t permanent fixtures. They represent recoverable opportunities that integrated lifecycle management can help resolve.
Now that these losses are on your radar, it’s time to act. Simplify patient interactions at every stage, from scheduling to follow-ups. Tools like automated reminders, same-day appointments, and telehealth options can improve engagement while boosting cash flow. For instance, automated appointment reminders have been shown to cut no-show rates by as much as 25%. Meanwhile, practices that adopt comprehensive revenue cycle management technology often see cash flow improvements of 20–30% within just a year. And don’t underestimate the power of personalized communication – whether it’s through text, email, or phone – to make patient engagement more efficient and effective.
“Recovering missed revenue is not impossible anymore.” – Tebra
To turn these gaps into gains, focus on the numbers. Keep an eye on denial rates, billing efficiency, days in accounts receivable, and revenue per patient encounter. These metrics can pinpoint where revenue is slipping through the cracks and guide your strategy to address those areas. Building on the earlier discussion of integrated lifecycle management, it’s clear that streamlined processes, better documentation, and automated payment tracking are key to recovering lost revenue.
Start small – whether it’s implementing automated reminders, offering more flexible scheduling, or tightening up billing accuracy. Each step builds on the last, turning missed opportunities into recovered revenue and, ultimately, better patient care.
FAQs
How does integrated patient lifecycle management help reduce no-shows?
Additionally, predictive tools play a key role by identifying patterns such as frequent rescheduling or overdue balances. This enables providers to step in early with targeted outreach to prevent cancellations. Offering flexible options like telehealth further reduces barriers like transportation or scheduling conflicts. The result? Fewer missed appointments, more consistent revenue, and less stress for healthcare staff.
What causes revenue loss in behavioral health practices?
Delayed or incomplete payments also play a major role. Issues like denied insurance claims or slow payment collection not only drag out the payment cycle but also increase the risk of accumulating bad debt. These financial setbacks are compounded by operational inefficiencies, as staff are forced to spend considerable time on tasks like rescheduling appointments, chasing overdue payments, and managing underutilized resources. To combat these problems, prioritizing proactive patient engagement and streamlining revenue-cycle management is essential for reducing losses and maintaining financial stability.
How do billing inefficiencies affect healthcare providers’ revenue?
The impact doesn’t stop at lost billable hours. When a patient skips an appointment, the provider still has to cover staffing and operational costs, creating a double hit – no income from the visit, yet expenses remain the same. On top of that, delays in submitting claims, poor handling of denials, and disjointed collection processes all contribute to further revenue losses. These issues underscore the importance of having a strong patient lifecycle management system in place to help safeguard margins and enhance financial outcomes.




