Disconnected tools are holding behavioral health organizations back. Even with advanced EHR software, scheduling apps, and billing platforms, growth stalls because these systems don’t communicate effectively. This leads to wasted time, manual workarounds, and errors that hurt both staff efficiency and patient care. Adding more tools only compounds the problem, creating more silos and complexity.
The solution? Connect your existing systems. Integrated platforms streamline data flow, reduce duplicate tasks, and improve decision-making with real-time insights. For example:
- Staff Efficiency: Automating workflows can save thousands of hours annually.
- Patient Care: Seamless data sharing ensures better coordination and outcomes.
- Financial Performance: Linking clinical and billing systems reduces errors and claim denials.
Organizations like GRAND Mental Health and Coleman Health Services have already seen major improvements – saving hundreds of hours and cutting documentation delays by days. By shifting to connected systems, behavioral health providers can simplify operations, improve care, and position themselves for sustainable growth.
How Disconnected Systems Block Growth
Fragmented Data and Workflows
When your EHR, payroll system, and billing platform don’t communicate, departments end up working in silos. For example, clinicians might document sessions in one system, but that data doesn’t automatically flow to billing. Meanwhile, HR tracks staff hours and credentials on a separate platform, leaving leadership in the dark about whether therapists are overbooked or underutilized unless they manually gather data from various sources.
This fragmentation forces staff to rely on outdated tools like spreadsheets and sticky notes for tasks that should be automated. Not only does this waste time, but it also increases the likelihood of costly errors. For patients moving between care settings, these disconnected systems can delay access to vital medication lists and treatment histories, leaving new care teams scrambling to piece together records manually.
The financial toll is hard to ignore. Behavioral health practices lose 10% to 20% of potential revenue due to preventable billing errors and claim denials. These issues arise because disconnected billing platforms can’t identify patterns in insurance rejections or automatically link clinical notes to claims. In one case, a behavioral health organization with over 90 service locations found that five manual reporting processes – spanning billing summaries, regional director reports, and census data – were eating up 1,194 staff hours each month. By automating these workflows, they estimated annual savings of $736,920 in staff time alone.
This lack of integration doesn’t just disrupt data flow – it drains staff efficiency and compromises the quality of care patients receive.
Effects on Staff Productivity and Patient Care
Disconnected tools don’t just bog down administrative tasks – they also directly impact clinician productivity and patient experience. Clinicians, for instance, switch tasks 1.4 times per minute, which adds up to over an hour of lost patient care every day.
Leadership struggles too. Without integrated systems, even basic reports – like analyzing payer mix by program or comparing staff productivity to caseloads – require time-consuming manual effort. Dr. Omar Fattal, System Chief of Behavioral Health at NYC Health + Hospitals, summed it up perfectly:
“You cannot do this work without data. You cannot fly this plane completely blind”.
When workforce data is siloed in HR systems and clinical data is locked in the EHR, managers can’t quickly pinpoint which teams are overburdened or which programs may be underperforming.
Patients also bear the brunt of these inefficiencies. Fragmented systems often force them to repeat their treatment histories with every new provider, which can be frustrating and lead to higher dropout rates. When care coordination relies on manual processes instead of automated data sharing, critical information often gets lost, and patient outcomes inevitably suffer. To mitigate these risks, organizations are increasingly adopting digital interventions to maintain engagement and support recovery goals.
Why More Tools Make the Problem Worse
The Real Cost of Too Many Tools
Adding more software to fix disconnected systems often backfires for behavioral health organizations. Instead of solving the problem, it creates “integration sprawl” – a messy web of systems trying to communicate directly with each other without a central framework. This setup makes the tech stack fragile. A simple update to one platform can disrupt workflows, delay payroll, or block access to critical reports.
The financial toll goes beyond just paying for software licenses. When multiple platforms handle data differently, it leads to “data drift.” For instance, if an EHR formats patient names one way but the billing system does it another way, someone has to step in and manually fix the discrepancies. This misalignment makes it nearly impossible to use data effectively for growth or improving patient care. Over time, leadership starts doubting the data altogether, making fast, confident decisions a real challenge. The result? Higher costs and slower progress.
Lost Opportunities for Data-Driven Growth
Disconnected systems don’t just cost money – they also get in the way of using real-time data for strategic decisions. As Josh Clark, Vice President of Quality & Safety Operating Systems at the Institute for Healthcare Improvement, explains:
“Most health systems do not have a technology gap. They have an integration gap.”
The problem isn’t a lack of data; it’s that the data is trapped in silos, making it impossible to get a full picture of operations. Many systems only provide outdated information, often two to three months old. While that might work for board meetings or compliance reports, it’s useless for making quick clinical decisions or spotting growth opportunities in real time.
Without integrated systems, even basic strategic questions remain unanswered. Which programs generate the most profit? Which payers frequently deny claims? Are your top-performing clinicians overbooked while others have open schedules? As Clark points out:
“Our frontline folks don’t have the data that they need to make decisions to drive care when they need it”.
This lack of integration becomes even more problematic as behavioral health shifts toward value-based contracting and measurement-informed care. Starting January 1, 2026, CARF accreditation standards will require organizations to show how they collect and use outcome data in treatment decisions. Meeting these standards will be nearly impossible if data remains scattered across disconnected platforms.
The Benefits of Connected Systems
Connected systems address the challenges of siloed data by offering immediate and practical advantages. By integrating tools like clinical EHR, payroll, billing, and outcome measurement systems, these solutions provide a single source of truth for all organizational data. This eliminates the need for leaders to reconcile conflicting reports or wait for manual data compilations. Instead, they gain real-time visibility into critical metrics, such as bed capacity, clinician performance, intake bottlenecks, and billing delays.
This unified approach also enhances reporting capabilities far beyond what standard EHRs can offer. Organizations can quickly analyze payer mix by program, evaluate staff productivity against caseloads, and monitor grant deliverables. These insights are crucial for identifying high-performing programs and staying competitive in value-based contract opportunities. Leadership can now base decisions on current, reliable data rather than outdated reports.
But the benefits don’t stop at smarter decision-making – connected systems also transform daily operations.
Unified Data for Faster Decisions
With connected systems, organizations achieve a single source of truth, integrating data from various tools like clinical EHR, payroll, and billing systems. This unified approach eliminates the headaches of reconciling conflicting reports or waiting for manual data updates. Leaders gain real-time visibility into key operational metrics, such as bed availability, clinician performance goals, and billing delays.
Additionally, this integrated data unlocks powerful reporting capabilities. For example, organizations can analyze payer mix by program, assess staff productivity relative to caseloads, and track the progress of grant deliverables. These insights are invaluable for identifying successful programs and competing for value-based contracts. Instead of relying on outdated snapshots, leadership can make informed decisions using up-to-the-minute data.
Better Experience for Staff and Patients
Integration doesn’t just benefit decision-makers – it also enhances the daily experience for staff and patients. For clinicians, connected systems simplify workflows by automatically linking assessments, treatment plans, and progress notes, significantly reducing repetitive data entry. This ensures clinical consistency while freeing up time for patient care.
Patients also benefit from seamless transitions between care levels. When moving from residential to outpatient care, for instance, connected systems ensure that medication lists, treatment histories, and care plans are transferred automatically. This eliminates the risk of dangerous gaps in coordination caused by fragmented data. Field-based teams also see improvements, as mobile documentation syncs automatically when connectivity is restored, keeping workflows uninterrupted regardless of location.
On the administrative side, connected platforms streamline the revenue cycle by linking clinical activities directly to billing and claims. This automation reduces manual charge entry, shortens charge lag times, and minimizes insurance denials due to inconsistent data. The result? Less administrative burden for staff, quicker reimbursements for the organization, and more room for growth.
How ContinuumCloud Connects Your Systems 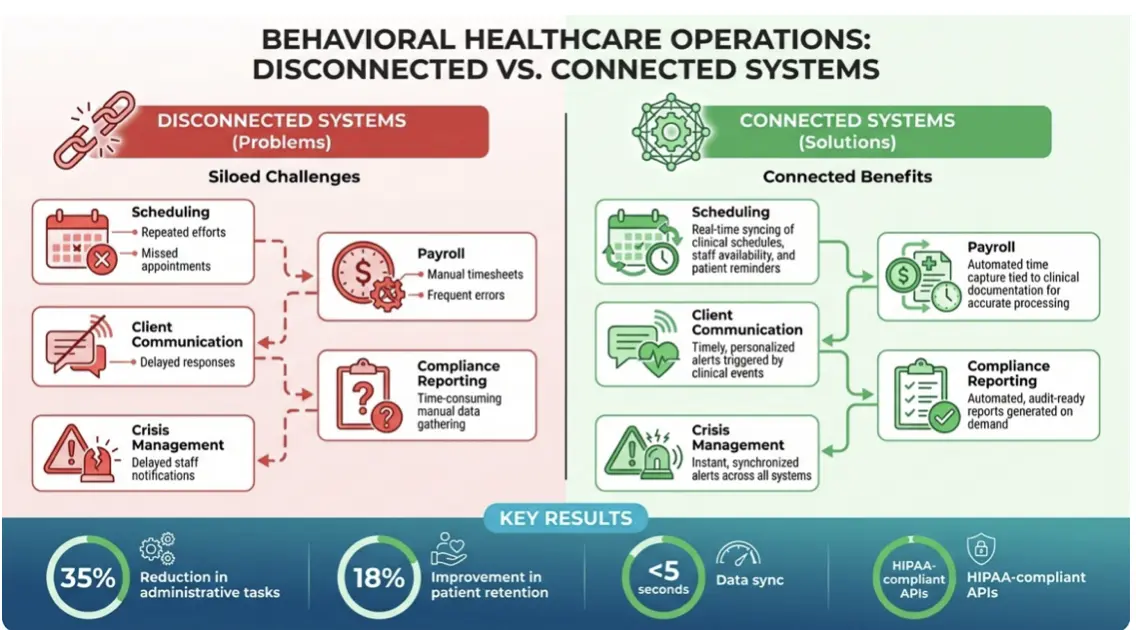
ContinuumCloud makes sure your systems work together seamlessly, eliminating the frustrations of disconnected tools.
By integrating clinical, workforce, and patient engagement operations, ContinuumCloud breaks down silos. It brings together clinical documentation, treatment planning, revenue cycle management (Welligent), workforce management, payroll and scheduling (DATIS), and patient engagement (CaredFor) into a single, unified platform.
Here’s how it works: when a clinician logs a session in Welligent, that data automatically flows to DATIS for billing and payroll calculations. At the same time, it updates CaredFor to send personalized follow-up messages to patients. This streamlined process saves time and reduces errors.
Integration Across Clinical, Workforce, and Patient Systems
The platform uses HIPAA-compliant APIs and single sign-on to keep data in sync across all systems in real time – typically in under five seconds. For example, when a patient’s appointment is scheduled in Welligent, DATIS adjusts staff assignments based on availability and credentials, while CaredFor sends appointment reminders and pre-visit surveys.
Organizations have already seen the difference. GRAND Mental Health, starting in January 2024, saved over 400 staff hours in just six months by integrating their clinical, workforce, and engagement systems. Their AI-powered documentation completed more than 80% of progress notes automatically, with data flowing effortlessly between systems.
Similarly, Coleman Health Services implemented the platform in May 2024. They reduced documentation time by 70% and cut note submission delays from five days to just 1.5 days. Clinical staff reported 92% satisfaction with the new workflow. Bob Bates, CEO of ContinuumCloud, highlighted the impact:
“Together we’re giving clinicians their time back while ensuring defensible, compliant documentation.”
Comparing Disconnected vs. Connected Approaches
The difference between working with siloed tools versus an integrated platform is clear in day-to-day operations. Here’s a closer look:
|
Workflow Area |
Siloed Challenges |
Connected Benefits |
|
Scheduling |
Repeated efforts, missed appointments |
Real-time syncing of clinical schedules, staff availability, and patient reminders |
|
Payroll |
Manual timesheets, frequent errors |
Automated time capture tied to clinical documentation for accurate processing |
|
Client Communication |
Delayed responses |
Timely, personalized alerts triggered by clinical events |
|
Compliance Reporting |
Time-consuming manual data gathering |
Automated, audit-ready reports generated on demand |
|
Crisis Management |
Delayed staff notifications |
Instant, synchronized alerts across all systems |
Organizations using ContinuumCloud’s integrated platform often cut administrative tasks by 35% and improve patient retention by 18%, thanks to enhanced engagement. The platform also meets Meaningful Use III and ONC-ACB certification standards, ensuring top-tier security, interoperability, and clinical quality.
Steps to Move from Siloed to Connected Systems
Shifting from isolated systems to a unified platform is a process that requires careful planning. Breaking it into three manageable steps can help smooth the transition. ContinuumCloud supports each phase, addressing integration challenges and simplifying your operations.
Identify Gaps in Your Current Systems
Begin by mapping out areas where data flow is interrupted. Look closely at how information moves – or doesn’t – between your clinical, scheduling, payroll, and communication tools. Pinpoint where duplicate data entries or delays are slowing things down.
For example, if clinicians have to log sessions in one system and then manually record their time for payroll in another, that’s a clear gap. Similarly, if staff must manually extract data to send appointment reminders, it’s another sign of a disconnect. These inefficiencies reveal where integration is most needed to reduce frustration and improve workflow.
Adopt Platforms That Work Together
Choose platforms that automatically share data using HIPAA-compliant APIs. Look for systems that seamlessly integrate clinical, workforce, and patient engagement functions.
It’s important to select EHR software designed specifically for behavioral health, rather than repurposed from general healthcare solutions. Specialized platforms offer features like DSM-5 templates, one-click group therapy notes, and “my eyes only” settings for sensitive information. These tools align with your unique workflows and compliance needs, which generic systems often fail to address.
Use Data to Drive Improvement
Once your systems are connected, take advantage of real-time data to enhance operations. Unified platforms provide immediate insights into patterns like no-shows, documentation delays, and staffing shortages.
For instance, if data shows that sending appointment reminders 48 hours in advance reduces no-shows, you can fine-tune your messaging schedule. If certain times of day see documentation bottlenecks, you can redistribute workloads or offer targeted training. These connected systems eliminate the need for manual data collection, allowing you to act on insights quickly and effectively.
Conclusion
The challenges outlined here highlight a key takeaway: meaningful progress in behavioral health hinges on effectively connecting the tools you already have. Adding more systems isn’t the answer. Fragmented setups lead to silos, duplicate efforts, and a lack of crucial, real-time insights. The real solution lies in integration.
ContinuumCloud takes a unified approach to break down these barriers, bringing together clinical documentation, workforce management, and patient engagement into unified behavioral health software. The results speak for themselves: Coleman Health Services cut provider documentation time by 70% and reduced note submission delays from five days to just 1.5 days, while GRAND Mental Health saved over 400 staff hours in just six months.
“Together we’re giving clinicians their time back while ensuring defensible, compliant documentation.” – Bob Bates, CEO, ContinuumCloud
These outcomes go beyond operational efficiency – they set the stage for long-term success. Connected systems free up staff to focus on what matters most: patient care. They also help prevent compliance risks and costly denials through real-time audits. Leadership gains access to the data needed to monitor performance and scale initiatives effectively. Integrating systems doesn’t just streamline operations – it fuels growth.
Transitioning from disjointed tools to connected systems takes effort, but the benefits are undeniable: improved patient outcomes, reduced staff burnout, and better financial performance. By embracing integration, behavioral health organizations can unlock new levels of efficiency, enhance care delivery, and position themselves for sustained growth.




