Turnover in behavioral health is alarmingly high, with rates often exceeding 50%, creating a crisis for organizations and the patients they serve. The constant staff churn disrupts care, drives up costs, and burdens remaining employees. Outdated HR systems are a major culprit, failing to meet the industry’s unique demands like credential tracking, compliance, and efficient onboarding. These inefficiencies increase administrative workloads, delay hiring, and contribute to burnout.
Modern HR and HCM systems offer solutions by automating routine tasks, integrating disconnected tools, and providing real-time insights to improve employee retention. Organizations that invest in better HR technology can reduce turnover, improve staff satisfaction, and ensure consistent, high-quality care for their clients.
How HR Systems Contribute to Behavioral Health Turnover
Why Legacy HR Systems Don’t Work for Behavioral Health
Standard HR platforms often fall short in meeting the unique demands of behavioral health organizations. These systems struggle to manage the rigorous credentialing requirements that are a cornerstone of the industry. Certifications, ongoing training, and license renewals require constant tracking and updates. Without automated solutions, HR teams are left to manually oversee these tasks, significantly increasing the risk of compliance issues.
Another problem with legacy systems is their focus on individuals rather than roles. When a therapist or counselor leaves, the system often loses track of the position itself. This creates gaps in budgeting and disrupts approval workflows. In contrast, position-based systems tie budgets and responsibilities to roles rather than individuals, preserving organizational structure even during staff transitions.
For over 25 years, behavioral health organizations have turned to specialized human capital management tools because generic software simply doesn’t address their specific challenges. However, many of these organizations are still stuck with outdated platforms that fail to align with their operational realities. These legacy systems contribute to broader administrative inefficiencies that further strain resources.
How Disconnected Systems Increase Administrative Work
The challenges of legacy systems are compounded when HR functions are spread across multiple disconnected platforms. Payroll, scheduling, and talent management often exist in silos, forcing HR teams to toggle between systems and reconcile conflicting data manually. This inefficiency not only wastes valuable time but also increases the likelihood of errors. A study in Oregon revealed that 13 out of 24 participants identified coding and billing limitations as a major source of frustration.
“Nobody enjoys constantly switching between systems to piece together all the necessary information, increasing user frustration as conflicting data emerge.”
The administrative burden doesn’t stop with HR teams – it spills over to clinicians as well. Documentation requirements in behavioral health often exceed what can reasonably be completed during a standard workweek. Disconnected systems make it harder to track client records and retrieve necessary documents promptly. When funding comes from multiple sources with differing documentation standards, staff are forced to spend hours reconciling records, which can delay much-needed funding.
These inefficiencies also lead to delayed onboarding processes, leaving existing staff to shoulder overwhelming caseloads for extended periods. This “caseload creep” often drives employees to quit, creating a vicious cycle of turnover. One county behavioral health director summed up the frustration well: “How do we have the experience of our workforce be directed at supporting community members, rather than meeting all of the administrative requirements? This work is so hard, and those requirements on top of it [are] wearing our folks down”.
The True Cost of Turnover in Behavioral Health
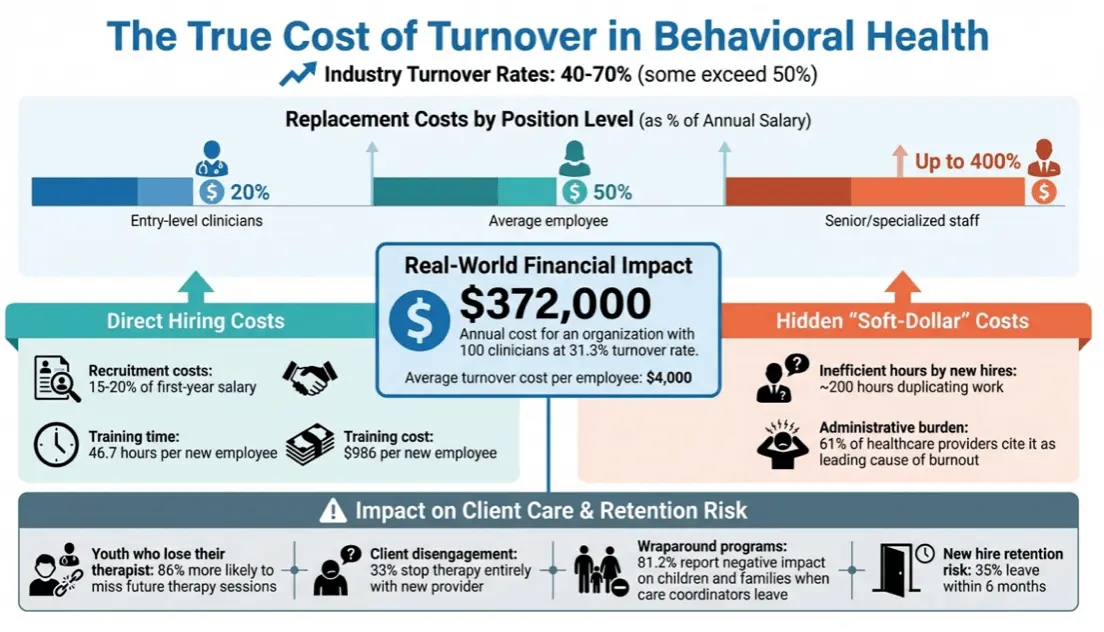
The Financial Impact of Turnover in Behavioral Health Organizations
Financial Costs: Recruitment, Training, and Lost Productivity
Turnover in the behavioral health field comes with a hefty price tag. On average, replacing a single employee costs about 50% of their annual salary. For entry-level clinicians, these costs typically begin at 20% of their salary, while for highly specialized or senior-level staff, the figure can climb up to a staggering 400%. To put this into perspective, an organization with 100 clinicians and a turnover rate of 31.3% could face an annual financial burden of around $372,000.
The financial toll includes a mix of direct and indirect expenses. Recruitment costs alone usually range from 15% to 20% of the new hire’s first-year salary, with the average cost per hire hovering near $4,700. On top of that, training a new employee takes roughly 46.7 hours and costs about $986 in direct expenses.
But the hidden costs – often referred to as “soft-dollar” expenses – are just as impactful. For instance, new hires spend approximately 200 inefficient hours duplicating work as they navigate institutional processes. This learning curve creates a “productivity debt”, forcing existing staff to take on additional workloads, which can lead to burnout and, ultimately, even more turnover. High turnover also jeopardizes the implementation of Evidence-Based Practices (EBPs) by reducing the number of skilled staff and compromising the quality of care.
How Turnover Affects Client Care and Outcomes
The consequences of turnover extend far beyond financial losses – it directly impacts the quality-of-care clients receive. When clinicians leave, it disrupts the therapeutic relationships that are essential for effective treatment. For example, youth who lose their therapist are 86% more likely to miss a future therapy session, and about 33% disengage entirely from therapy with a new provider. This lack of continuity can significantly undermine treatment outcomes.
In Wraparound programs, turnover has particularly damaging effects. A striking 81.2% of respondents reported that losing care coordinators negatively impacts children and families. Additionally, 66.7% observed increased workloads for remaining staff, 52.1% cited greater strain on supervisors, and 51.8% noted a decline in care quality. The departure of experienced providers also leads to a loss of institutional knowledge, making it harder to maintain and expand evidence-based practices.
This revolving door of staff creates an unstable work environment, which becomes a systemic obstacle to meeting growing community needs. High turnover limits an organization’s ability to scale its services and undermines its capacity to deliver consistent, high-quality care.
How Modern HR Systems Reduce Turnover
What Integrated HR Systems Offer
Modern HCM platforms bring together recruiting, onboarding, payroll, talent management, and timekeeping into a single, cohesive system. By uniting these functions, they eliminate the headaches of managing multiple disconnected tools, cutting down on paperwork and allowing teams to focus more on client care.
These systems also take over tedious compliance tasks that often weigh down behavioral health teams. Things like license renewals, certification tracking, and background checks are handled automatically. Managers receive timely alerts before credentials expire, ensuring the organization stays audit-ready without constant manual follow-up. On top of that, position control features help leaders align staffing levels with clinical needs and budget constraints. This is especially crucial as nearly 66% of behavioral health organizations plan to expand their services in 2024.
Recruitment tools designed with mobile users in mind allow organizations to connect with candidates via text, making the hiring process more accessible and engaging. Once new hires come on board, a streamlined onboarding process guides them through their first 90 days – a period when retention is especially vulnerable, as about 35% of new hires in behavioral health leave within six months. These systems also integrate scheduling with HR data, giving managers real-time insight into workloads. This helps distribute tasks more evenly and prevents burnout, a key factor in turnover. By combining these features, modern HR platforms not only simplify operations but also set the stage for stronger retention strategies.
How Better HR Technology Improves Retention
Modern HR technology goes beyond basic integration to actively support employee retention. Advanced systems use real-time data – such as attendance records and weekly pulse surveys – to spot early signs of disengagement, giving managers a chance to address concerns before they escalate.
Instead of relying on outdated annual surveys, these platforms collect feedback through automated weekly pulse surveys. This approach captures how employees feel in real time, enabling managers to tackle small issues before they turn into bigger problems. Additionally, these systems track key performance metrics, making it easier for managers to recognize and reward top performers. Acknowledging achievements fosters a sense of value among staff, which can go a long way in retaining talent.
Turnover in the behavioral health industry is costly, averaging $4,000 per employee, with some organizations experiencing rates as high as 70%. Modern HR tools help break this cycle by providing constant visibility into hiring needs and employee engagement. This reduces the strain on existing staff, leading to a more stable workforce. In turn, organizations can deliver better client outcomes and redirect savings from reduced turnover into growth and improved services.
Conclusion: Reducing Turnover with Better HR Systems
Turnover in behavioral health is a significant challenge, costing organizations an average of $4,000 per employee. With turnover rates ranging between 40% and 70%, it disrupts the continuity of care that clients rely on. Adding to the problem, 61% of healthcare providers identify administrative overload as a leading cause of burnout. Outdated systems – packed with disconnected tools and manual processes – only worsen the strain. Tackling this issue calls for targeted HR solutions.
The key to addressing these frustrations lies in adopting HR technology tailored specifically to the needs of behavioral health organizations. Modern EHR software streamlines routine tasks like documentation, admissions, and scheduling, while mobile recruitment tools help eliminate inefficiencies that contribute to turnover. Additionally, when nearly half of employees (48%) say they’re more likely to stay with organizations that act on their feedback, tools like automated pulse surveys and data-driven recognition become essential. These features not only improve retention but also create a more supportive and engaged work environment.
“How do we have the experience of our workforce be directed at supporting community members, rather than meeting all of the administrative requirements? This work is so hard, and those requirements on top of it [are] wearing our folks down.” – County behavioral health director
Integrated HR systems offer a way to break the cycle of chronic turnover. By reducing the administrative burden on clinicians and implementing tools like 90-day onboarding tracking to address disengagement early – when employees are most at risk of leaving – organizations can build a more stable workforce. For behavioral health providers looking to expand services, investing in modern HR technology is essential. It not only ensures consistent, high-quality care but also creates opportunities to reinvest in improving care delivery.
FAQs
How do outdated HR systems lead to high turnover in behavioral health organizations?
When staff are stuck wrestling with outdated systems instead of focusing on their primary duties, morale takes a hit. This can lead to lower job satisfaction and, ultimately, higher turnover rates. For behavioral health organizations, adopting streamlined, modern HR solutions isn’t just a nice-to-have – it’s essential for easing workplace stress, boosting efficiency, and keeping employees on board.
What are the must-have features in HR systems to reduce turnover in behavioral health organizations?
Using advanced analytics, organizations can monitor turnover patterns and pinpoint roles at higher risk for attrition. Tools for flexible scheduling can help employees achieve better work-life balance, which is critical in high-stress environments. Integrating payroll, benefits, and position-control systems ensures accuracy and builds trust, while exit and stay interview tools offer valuable feedback to address underlying issues. Together, these features help create a workplace where employees feel supported, engaged, and less likely to experience burnout.
How does employee turnover affect the quality of care in behavioral health organizations?
Frequent changes in personnel can also slow down or complicate the adoption of evidence-based practices, reducing the overall effectiveness of care. Keeping skilled and experienced staff on board is key to delivering steady, high-quality support to clients.




