Behavioral health organizations are grappling with workforce shortages, high turnover, and financial pressures. Labor costs often dominate their budgets, but many lack systems to connect staffing decisions with financial impact. Enter position control: a strategy that focuses on managing roles rather than individual employees.
This approach keeps positions active in systems – even when vacant – ensuring budgets, qualifications, and funding details remain intact. It helps organizations prioritize recruitment, control labor costs, and maintain service levels. For example, it can reduce overtime expenses and reliance on costly temporary staff, while also improving budget accuracy.
Key takeaways:
- Position control tracks roles, not just employees, providing clarity on vacancies and costs.
- It supports better workforce planning by aligning staffing needs with financial realities.
- Organizations using position control report reduced costs, improved retention, and streamlined operations.
With workforce shortages projected to worsen, position control offers a practical solution to stabilize finances and meet rising care demands. It’s not just a tool – it’s a step toward smarter, more efficient workforce management.
The Behavioral Health Workforce Crisis and Its Financial Impact
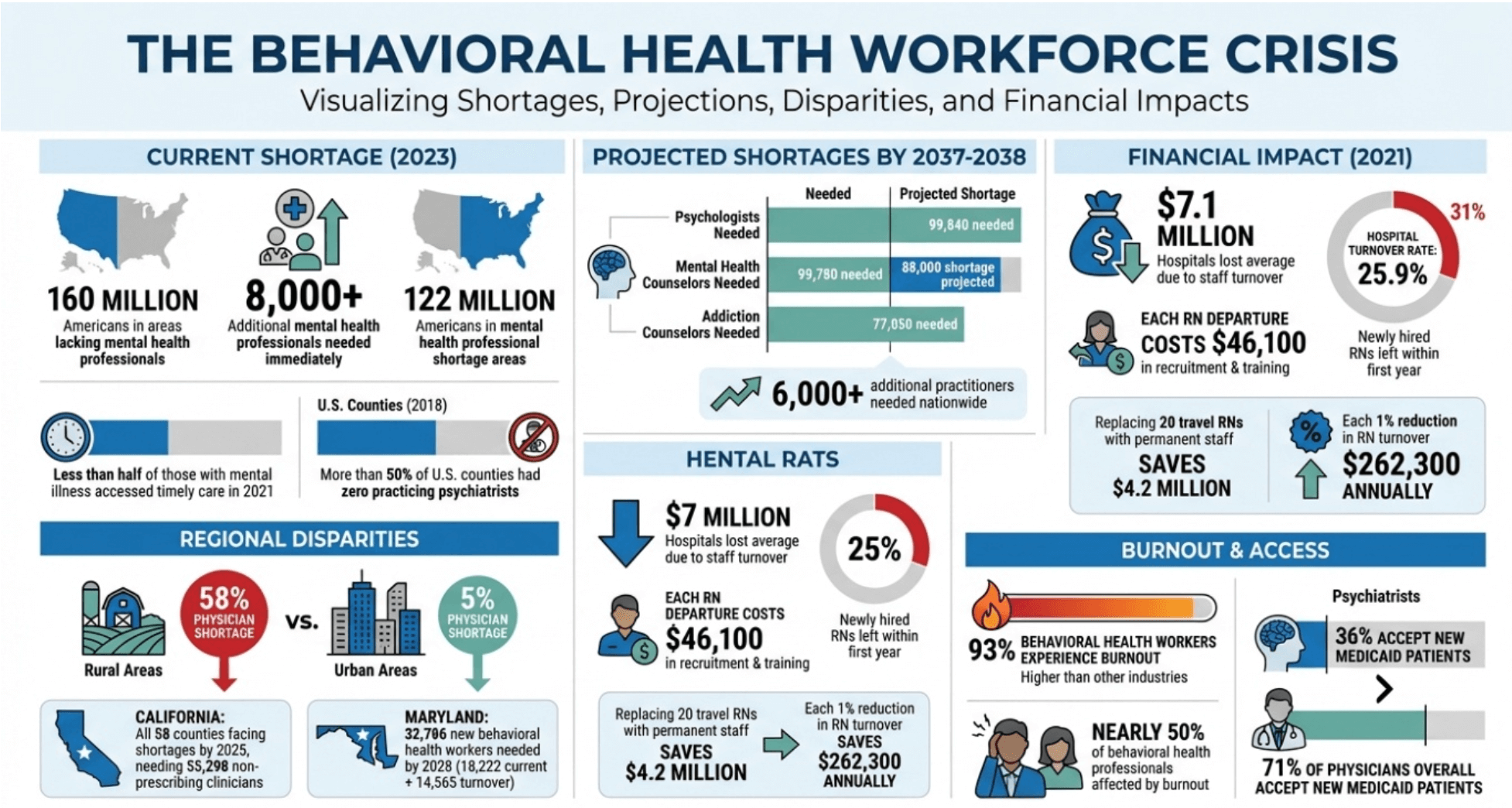
Behavioral Health Workforce Crisis: Key Statistics and Projected Shortages
Understanding the Behavioral Health Workforce Shortage
As of March 2023, a staggering 160 million Americans lived in areas lacking enough mental health professionals. At that time, the U.S. needed over 8,000 additional mental health professionals to meet demand. The situation is even more alarming in rural areas – back in 2018, more than half of all U.S. counties didn’t have even one practicing psychiatrist.
Looking ahead to 2038, the numbers paint an even grimmer picture. The country is projected to face shortages of 99,840 psychologists, 99,780 mental health counselors, and 77,050 addiction counselors. Rural areas, or nonmetropolitan regions, will feel this crisis most deeply, with a predicted 58% shortage of physicians compared to just 5% in urban areas. These gaps represent millions of people who may struggle to find the care they urgently need.
“The scarcity of behavioral health professionals is undermining people’s ability to get timely care. This is reinforced by historical underinvestment in behavioral health care by public insurance programs… private insurers, and employers.”
– Nathaniel Counts, Chief Policy Officer, Kennedy Forum
In 2021, fewer than half of those experiencing mental illness were able to access timely care. This mismatch between need and availability forces organizations to make tough decisions, often leaving critical positions unfilled for long periods as they search for qualified professionals.
How Workforce Instability Affects Finances
The shortage of mental health professionals doesn’t just limit access to care – it also creates major financial headaches for healthcare organizations. Recruitment and operational costs skyrocket, putting a strain on budgets. For example, in 2021, hospitals lost an average of $7.1 million due to staff turnover, with each registered nurse (RN) departure costing around $46,100 in recruitment and training. Nationwide, hospital turnover rates hit 25.9% that year, and 31% of newly hired RNs left within their first year.
When positions remain vacant, organizations often face a tough choice: either reduce services or rely on costly temporary staff. Many choose the latter to maintain revenue. To put it into perspective, replacing 20 travel RNs with permanent staff could save a hospital an average of $4.2 million. Premium labor costs, however, eat into operating margins and destabilize financial planning.
Vacancies also lead to lost billable hours, directly impacting revenue. For every percentage point reduction in RN turnover, organizations can save $262,300 annually. Yet, less than half of hospitals have measurable retention goals in place to track and improve these numbers. Without clear systems to monitor staffing – whether positions are filled, vacant, or temporarily staffed – many organizations fail to grasp the full financial impact of workforce instability.
Adding to these challenges are low insurance reimbursement rates. Only 36% of psychiatrists accept new Medicaid patients, compared to 71% of physicians overall. This gap has given rise to “insurance ghost networks”, where providers are listed in directories but don’t actually see patients, further restricting access. These financial and operational pressures highlight the urgent need for better workforce planning tied to sound financial strategies.
How Position Control Connects Workforce Planning and Financial Stability
Improving Workforce Planning with Position Control
Position control offers a focused way to tackle workforce challenges by shifting attention from tracking individual employees to managing specific roles. This approach is particularly useful in behavioral health, where turnover is high and staff often move between programs. Instead of centering on the person in the role, the position itself becomes the constant. Each role is tied to set attributes – such as salary, credentials, department, and funding source. For instance, when a therapist leaves, the system retains all the critical data tied to that position, including cost and qualification details.
This structure allows leaders to create realistic staffing models using full-time equivalent (FTE) data. They can analyze positions in relation to patient caseloads and budget constraints. For example, an organization might decide to fill a vacant psychiatrist role with two part-time clinicians, balancing flexibility with financial limits. Considering that over 122 million Americans live in areas with a shortage of mental health professionals – and with a projected shortfall of 88,000 mental health counselors by 2037 – this level of precision helps organizations avoid the pitfalls of understaffing, which can hurt revenue, or overstaffing, which can strain budgets.
Position control also provides real-time insights into which roles are filled, vacant, or temporarily staffed. This makes it easier for leaders to pinpoint and address scheduling gaps, especially in high-demand areas like child mental health or rural services. In California, for example, all 58 counties are expected to face behavioral health shortages by 2025, with a need for 55,298 additional non-prescribing clinicians. With a centralized view of staffing, organizations can strategically allocate limited resources to where they’re needed most.
Using Position Control to Maintain Budget Discipline
In addition to improving staffing accuracy, position control plays a key role in managing labor costs – the largest expense for behavioral health organizations. By organizing workforce data around positions rather than individuals, the system offers real-time dashboards that compare budgeted versus actual labor spending. This helps finance teams forecast costs more accurately, model different pay scenarios, and catch potential budget overruns early.
Position control also enforces discipline through approval workflows. Before a position can be posted or filled, it must go through designated approvals from HR and finance. This process prevents unplanned hiring that could disrupt budgets. As Dylan Souza, VP of Marketing at ContinuumCloud, puts it:
“The visibility that Position Control provides helps prevent the all-too-common issue of overhiring. In a Position Control system, open positions must be approved before filling them”.
By automating the oversight of roles, shifts, and compliance requirements, position control cuts down on administrative inefficiencies. Tasks like manually tracking open positions or handling overtime approvals become streamlined. This efficiency is especially important in light of Maryland’s projected need for 32,786 new behavioral health workers by 2028. Every hour saved on administrative tasks can be redirected to critical efforts like recruitment and retention.
Position Control in Practice
Behavioral health organizations have reported notable cost savings thanks to position control. Darcy Dibble, CFO of The Arc Otsego, highlighted its impact:
“It’s saved us a lot of money in the long run. It’s our best technology decision”.
The organization credits position control with curbing costs by preventing unauthorized hires and providing clear visibility into labor expenses across various programs. Similarly, healthcare systems facing challenges like high regulation, frequent turnover, and tight budgets have used position control to reduce overtime costs by 20–30% through data-driven shift management.
For organizations undergoing mergers or scaling operations, position control also simplifies workforce alignment. It helps define overlapping roles clearly and ensures workforce planning stays aligned with strategic goals, all while avoiding cost overruns. These outcomes highlight how position control serves as a bridge between effective staffing strategies and financial stability.
How to Implement Position Control in Behavioural Health Organizations
Creating a Complete Position Inventory
The first step in position control is building a thorough inventory of all roles within your organization. Think of it as focusing on the “seat” rather than the “sitter.” Even if a therapist leaves, the position itself remains intact in your system, retaining critical details like FTE value, salary range, required credentials, cost center, and funding source.
Start by conducting a baseline audit that compares your payroll data with your approved budget. This process can uncover “ghost” positions – unbudgeted hires that may be consuming resources without proper oversight. Once identified, standardize job titles to reduce redundancies and assign each position a unique identifier. This makes it easier to track long-term trends like turnover rates and recruitment costs.
For behavioral health organizations, it’s essential to include specific licensure requirements for each role – whether it’s an LCSW, LPC, or BCBA. This ensures compliance with state regulations and payer requirements. Clearly map out funding sources, identifying whether positions are supported through general operations, grants like SAMHSA, or Medicaid reimbursements. Collaborate with clinical directors to define role competencies and caseload capacities. This ensures your inventory reflects the organization’s real-world needs, not just theoretical structures.
Connecting Position Control with Workforce and Financial Systems
Once your position inventory is complete, the next step is integrating this data with your workforce and financial systems. The goal is to create a unified platform where information flows seamlessly between HR, payroll, and finance – eliminating the need for manual data entry. Moving away from scattered spreadsheets and consolidating data into your Human Capital Management (HCM) or ERP system is key.
Building on the budget discipline established earlier, link your system to the general ledger. This allows for real-time comparisons between budgeted and actual salaries, hours, and FTEs. With this setup, finance teams can forecast costs more accurately and identify potential budget overruns early. As Tami Lewis-Ahrendt, COO at CenterPointe, explains:
“If you are a behavioral health nonprofit and you have complicated funding streams that require you to report information back to them on how you pay people and why you pay people, then there is not another tool on the market that can do for you what the e3 product can do for you”.
Leverage daily lost revenue reports to pinpoint which vacant positions are causing the most significant financial impact. This helps clinical and finance leaders prioritize recruitment efforts strategically. Your system should also accommodate the unique challenges of behavioral health, such as employees working across multiple programs, varying pay rates, and shift differentials. This reduces administrative burdens and streamlines operations.
Working with Cross-Functional Teams During Implementation
Implementing position control successfully requires collaboration across HR, clinical leadership, and finance. Begin with joint training sessions where all teams learn the system together. This shared learning builds a common understanding of how position control works and how it helps maintain operational stability, even during vacancies.
Establish a formal protocol for adding, modifying, or removing positions. This prevents “budget creep” by ensuring all changes undergo proper review by both HR and Finance. Configure the system so that approvals and requests automatically flow to the appropriate decision-makers when a vacancy arises, maintaining continuity in leadership.
Michelle Mong, CFO at Folium, Inc., underscores the organizational benefits of such systems:
“The main impact for the system has been time saved…Not just for payroll and HR, but for everyone”.
Regular budget comparisons at the position level help teams identify and address potential issues before the fiscal year ends. When everyone operates using the same real-time data, collaboration becomes more effective, reducing miscommunication about workforce capacity and financial constraints. This unified approach not only ensures smooth implementation but also lays the groundwork for evaluating the long-term impact of position control in the future.
Measuring the Impact of Position Control
Metrics to Track
Once position control is implemented, monitoring the right metrics is essential to evaluate its effectiveness. Position fill rates are a key indicator, reflecting the percentage of authorized roles currently staffed. This metric provides a clear picture of workforce stability. In behavioral health, where over 122 million Americans live in areas with a shortage of mental health professionals, maintaining strong fill rates is crucial for serving clients effectively.
Turnover rates are another critical metric, especially in behavioural health. Burnout affects nearly half of professionals in this field, driven by factors like work-related stress, low pay, and heavy caseloads. According to the National Council for Mental Wellbeing, 93% of behavioural health workers experience burnout at higher rates than other industries. By analyzing turnover rates by department and specific roles, organizations can identify positions that require immediate intervention to improve retention.
Time-to-fill critical roles is also a vital measure. This tracks how quickly key positions – such as psychiatrists, therapists, and case managers – are staffed, impacting both service capacity and client outcomes. Pairing this with metrics like labor costs per position, vacancy durations, and overtime hours helps pinpoint areas of overspending on temporary staffing and reveals service gaps. Together, these insights highlight operational inefficiencies while paving the way for financial improvements.
Financial Benefits of Position Control
Position control delivers measurable financial advantages in three primary areas. First, lower overtime costs are achieved by providing real-time visibility into staffing needs. Instead of making last-minute, reactive staffing decisions that drive up overtime expenses, organizations can balance full-time and part-time staff based on actual patient demand. This approach minimizes the costly reliance on emergency coverage during high-demand periods.
Reducing dependence on temporary staffing is another significant benefit. By optimizing the permanent workforce, organizations can avoid the high costs associated with per diem or contract clinicians. Additionally, improved budget accuracy prevents unchecked labor spending. Darcy Dibble, CFO at The Arc Otsego, highlights this financial impact:
“It’s saved us a lot of money in the long run. It’s been the best decision technology-wise that we’ve ever made”.
Beyond immediate cost savings, position control data also supports strategic workforce planning, ensuring financial stability for the future.
Using Position Control Data for Future Planning
Position control data plays a transformative role in preparing for predictable workforce changes. By tracking historical trends in turnover, retirement eligibility, and resignations by department, organizations can plan ahead for recruitment and retention needs. For instance, Maryland’s behavioral health sector identified the need for 18,222 current workers, plus an estimated 14,565 additional hires to address turnover from retirements and exits – figures that demand proactive planning.
Unlike traditional systems that focus solely on employees, position control maintains detailed records of positions. This ensures that essential role data remains intact even after staff turnover. With this information, organizations can quickly identify which roles require immediate attention and which can be filled through internal mobility or training programs. This forward-thinking approach not only ensures service continuity but also helps manage budgets effectively. Meeting the demand for over 6,000 additional practitioners nationwide becomes more achievable with such data-driven strategies. Rigorous tracking like this supports both immediate staffing needs and long-term financial planning.
Conclusion
The behavioral health workforce is facing an undeniable crisis. Millions of Americans live in areas with severe provider shortages, while many behavioral health professionals are grappling with burnout at rates higher than in most other industries. This has left organizations under immense pressure to stretch limited resources further than ever before. Unfortunately, traditional workforce management tools – like spreadsheets, reactive hiring practices, and manual tracking – simply aren’t equipped to handle the complexities of today’s behavioral health operations.
This is where position control changes the game. By establishing a structured, position-based system, organizations can connect workforce planning directly to financial stability. Instead of constantly reacting to staffing gaps or overspending on overtime and temporary workers, position control offers real-time visibility into every position, its costs, and its role in service delivery. This clarity leads to tangible results: reduced overtime costs and more accurate budgeting, which helps prevent runaway labor expenses.
But position control isn’t just about saving money. It provides a solid foundation for planning workforce changes, managing intricate funding streams, and maintaining service continuity – even during high turnover periods. This financial transparency sets the stage for implementing the strategic steps discussed earlier.
Beyond immediate cost benefits, position control empowers organizations to take a data-driven approach to future planning. For leaders in behavioral health, who are navigating both workforce shortages and tight budgets, position control offers a clear and actionable path forward. Start by auditing your current positions, integrating position control into your HR and financial systems, and focusing on key metrics like fill rates, role-specific turnover, time-to-fill for critical positions, and labor costs per role. These steps turn workforce challenges into opportunities for strategic improvement.
With the nation needing over 6,000 additional practitioners and 32,786 new workers in Maryland alone by 2028, the question isn’t whether you can afford to adopt position control – it’s whether you can afford not to. Position control bridges the gap between understanding your workforce needs and achieving the financial stability necessary to meet them consistently.
FAQ
How can behavioral health providers use AI for documentation without losing the personal touch in patient care?
To make the most of AI tools, it’s important to tailor them to fit specific workflows and provide consistent training for staff. Regularly evaluating how these tools perform and strictly adhering to patient privacy laws are also key to maintaining trust and delivering personalized care. By combining efficiency with empathy, providers can strike a balance that benefits both clinicians and patients.
What are the key steps to start using position control in a behavioral health organization?
Next, define key attributes for each position. These might include full-time equivalent (FTE) values, salary ranges, budget codes, and compliance requirements. These details remain tied to the position itself, ensuring consistency even as employees move in and out of roles.Afterward, upload this position data into your HCM or payroll system. This allows you to track headcount, monitor vacancies, and manage spending at the position level. It’s also helpful to set up an approval process for creating or reopening positions to ensure alignment with your organization’s financial goals and to avoid exceeding your budget.
Finally, assign employees to their designated positions and flag any open roles. This step not only clarifies recruitment priorities but also provides a clear overview of workforce needs. By following these steps, you’ll create a solid framework for managing finances and planning your workforce effectively.
How does position control help address workforce shortages and improve recruitment and retention?
Position control gives behavioral health organizations a clear, up-to-date view of all roles – both filled and vacant – helping leaders zero in on where recruitment efforts are most needed. By tying each position to budget approvals, labor cost projections, and compliance standards, it eliminates unnecessary openings and ensures hiring targets the roles that matter most. This level of clarity allows organizations to move quickly, speeding up job postings and approvals to secure top talent before competitors do.
Another advantage of position control is that it separates roles from individual employees. This makes it easier to reassign responsibilities or share roles without causing workflow disruptions during staff transitions. By standardizing key aspects like pay, workload, and training requirements, managers can tackle issues like burnout, allocate resources wisely, and focus on filling high-priority positions. This data-driven strategy not only reduces the time it takes to fill roles but also signals to potential hires that the organization is stable and well-organized – qualities that are especially appealing in areas facing workforce shortages.




