ACCELERATE 2026 is where behavioral health leaders will find solutions to today’s toughest challenges, including proving measurable outcomes, addressing workforce shortages, and navigating new regulations. Scheduled for September 8–11, 2026, in Orlando, Florida, this event focuses on actionable strategies across five key areas: improving client outcomes, optimizing operations, smarter workforce strategies, leveraging AI, and aligning with cutting-edge technologies.
Key Highlights:
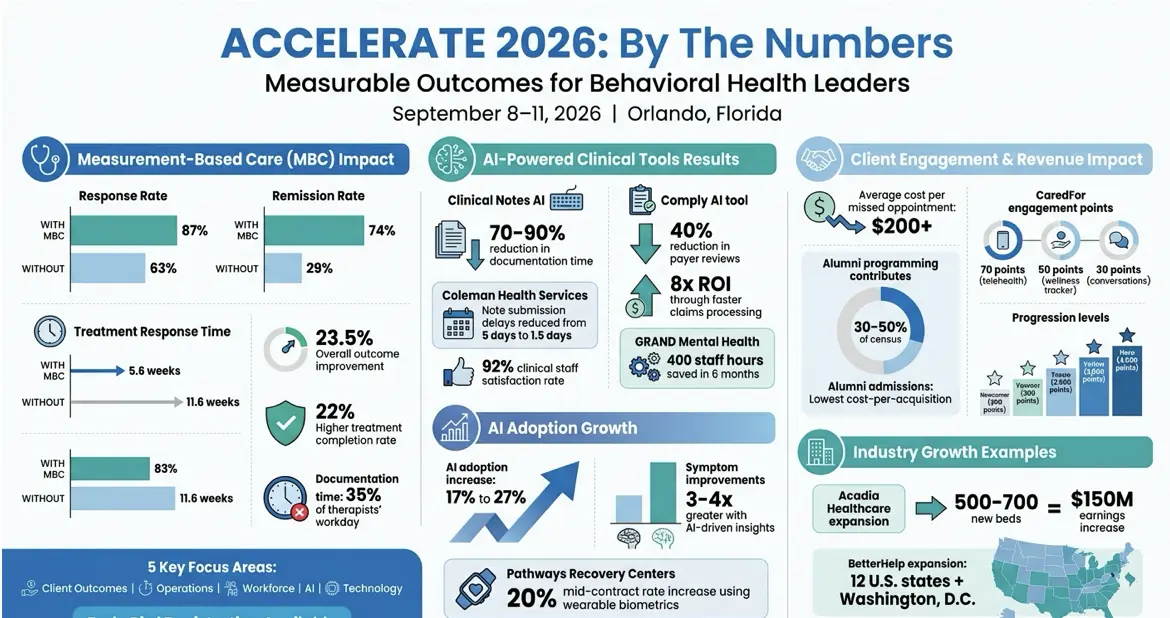
- Measurement-Based Care (MBC): Learn how to integrate tools like PHQ-9 and GAD-7 to improve outcomes by 23.5% and reduce treatment response times.
- AI-Powered Tools: Explore features like Clinical Notes AI (reduces documentation time by 70%) and real-time compliance auditing.
- Workforce Solutions: Discover how DATIS HCM reduces staffing inefficiencies with predictive analytics, mobile tools, and automated compliance tracking.
- Client Engagement: Use platforms like CaredFor to build online communities, reduce no-shows, and boost revenue through alumni programming.
- Product Roadmaps: Get an exclusive preview of updates for Welligent EHR, DATIS HCM, and CaredFor, including “Living” Treatment Plans that adapt as symptoms change.
This event is tailored to help leaders implement practical tools and strategies that improve outcomes, reduce costs, and drive growth in behavioral health. Don’t miss the opportunity to stay ahead of industry changes.
Actionable Strategies for Better Client Outcomes
ACCELERATE 2026 offers attendees practical, data-backed strategies they can put into action right away. The event focuses on two key areas: integrating Measurement-Based Care (MBC) into everyday workflows and enhancing client engagement with hands-on techniques.
Measurement-Based Care (MBC) Implementation
Measurement-Based Care involves using validated tools like the PHQ-9 for depression and GAD-7 for anxiety to guide treatment decisions. According to a 2025 study in Frontiers in Health Services, MBC significantly improves outcomes. The study revealed that MBC achieved an 87% response rate compared to 63% without it, a 74% remission rate compared to 29%, and reduced treatment response time from 11.6 weeks to just 5.6 weeks. Overall outcomes improved by 23.5%, and patients were 22% more likely to complete treatment successfully.
Despite its benefits, the biggest challenge remains implementation. Sessions at ACCELERATE 2026 will focus on overcoming this hurdle. Attendees will discover how to streamline assessments using digital tools that present routine evaluations as “Weekly Check-ins.” This approach not only engages clients but also cuts down on therapists’ documentation time, which currently takes up about 35% of their workday. Insights from the Child Development Institute‘s (CDI) MBC Accelerator Project will further guide participants on how to speed up MBC adoption within behavioral health organizations.
Once MBC is effectively in place, the next step is leveraging client engagement strategies to maximize its impact.
Improving Client Engagement
Pairing data-driven tools with stronger client interactions takes treatment outcomes to the next level. Workshops at the conference will show how to use visualized data trends – like color-coded severity levels and baseline comparisons – to make sessions more engaging. Providers will also learn how to integrate between-session tools, such as homework tracking and mood monitoring, to keep clients involved and reduce appointment no-shows. These techniques not only enhance the therapeutic relationship but also ensure subtle changes in a client’s progress are noticed early.
Combining MBC data with these engagement strategies creates a more complete picture of client progress. This holistic approach is not just clinically beneficial – it’s financially smart. Missed appointments cost practices over $200 on average, making these strategies a win-win for both providers and clients.
Welligent EHR Product Updates and Roadmap
ACCELERATE 2026 highlights how Welligent EHR is evolving to address operational challenges. The event will showcase its established features alongside exciting new developments.
Core Features on Display
The conference will spotlight Welligent’s core tools, which include caseload management, appointment scheduling, and revenue cycle management functions like eligibility verification and claims submission. The Welligent Connect patient portal will also take center stage, offering clients secure access to view records, complete intake forms, request prescription refills, and communicate with providers. Additionally, its mobile EHR capabilities allow for offline documentation that syncs automatically when back online. These tools form a solid foundation for the platform, with upcoming features designed to drive even greater efficiency.
Upcoming Features and Development Plans
The roadmap sessions will introduce AI-driven tools aimed at streamlining clinical workflows. One standout is Clinical Notes AI, which uses ambient listening to draft clinical notes automatically. This feature has the potential to reduce documentation time by up to 90%. For example, Coleman Health Services adopted this tool in May 2024 and saw impressive results: provider documentation time dropped by 70%, note submission delays decreased from five days to just 1.5 days, and clinical staff reported a 92% satisfaction rate with the platform.
“Together we’re giving clinicians their time back while ensuring defensible, compliant documentation.” – Bob Bates, CEO, ContinuumCloud
Another key feature is Comply, an AI-powered auditing tool that reviews documentation in real time to minimize denied authorizations. Organizations using Comply have reported a 40% reduction in payer reviews for level of care placement and an 8x return on investment through faster claims processing and improved compliance. For instance, GRAND Mental Health in Oklahoma automated over 80% of progress notes starting in January 2024, saving 400 staff hours within six months.
The roadmap also includes “Living” Treatment Plans, which automatically update as symptoms evolve. By integrating scoring assessments like the PHQ-9 and GAD-7, these plans provide real-time prompts to ensure diagnoses, treatment plans, and notes remain consistently aligned – helping maintain the “Golden Thread” of care.
Workforce Management Solutions with DATIS HCM
DATIS HCM is here to help teams tackle workforce challenges head-on. At ACCELERATE 2026, behavioral health organizations will see how this platform addresses critical issues like staffing shortages, turnover, and operational inefficiencies. By integrating recruiting, onboarding, payroll, and employee development into one cohesive system, DATIS HCM is designed specifically for behavioral health and human services.
Workforce Success Stories from Peer Organizations
One of the standout features of DATIS HCM is its Position Control tool, which focuses on managing positions rather than just employees. This approach ensures that staffing aligns seamlessly with available budgets and funding streams. Peer-led sessions will share real-world examples of how organizations have transformed their workforce operations with this feature.
“If you have complicated funding streams that require you to report information back to them… then there is not another tool on the market that can do for you what the e3 product can do for you.” – Tami Lewis-Ahrendt, Chief Operating Officer
DATIS HCM also streamlines recruitment through multi-channel job postings, automated candidate screening, and mobile-friendly applications, speeding up the hiring process. Retention gets a boost with features like self-service portals, pulse surveys, and employee recognition programs.
“If you’re in Health and Human Services, then this is the product. This is the way to go. Because they’ve already designed it according to that industry, and it just makes sense.” – Marion McLaurin, Senior VP of Human Resources
These stories provide a glimpse into how organizations are leveraging the platform to optimize their workforce operations, setting the stage for even more advancements in AI and automation.
AI and Automation in Workforce Operations
DATIS HCM is taking workforce management to the next level with AI-driven predictive analytics. These tools help organizations anticipate staffing needs, predict overtime, and identify potential turnover risks. Real-time analytics provide key HR metrics, including turnover rates, cost-per-hire, and time-to-fill, giving leaders actionable insights.
Compliance is another area where automation shines. The platform tracks license and credential expirations automatically, easing the administrative burden while ensuring organizations remain compliant with regulations.
For field-based staff, mobile-first tools make managing work easier than ever. Features like geofencing for clocking in and out, mobile schedule viewing, and instant access to pay stubs empower employees on the go. Add in drag-and-drop scheduling and open shift bidding, and managing 24/7 operations becomes far more efficient, helping supervisors avoid burnout.
Growth Strategies Using the CaredFor Platform
The CaredFor platform is designed to deepen client engagement, which in turn helps behavioral health providers grow and sustain revenue. At ACCELERATE 2026, you’ll discover how organizations are leveraging this tool to keep clients engaged during critical care gaps, transforming those connections into measurable growth.
Creating Online Client Communities
CaredFor offers a secure, HIPAA-compliant online space where patients, alumni, and families can connect and support one another. This setup reduces feelings of isolation and fosters a self-sustaining community that keeps clients engaged even after they leave treatment. The platform’s Contingency Management system adds an interactive element by gamifying positive behaviors. Users earn points for activities like attending telehealth sessions (70 points), completing wellness tracker entries (50 points), and starting conversations (30 points). As they accumulate points, members progress through five levels, from Newcomer (300 points) to Hero (4,500 points), keeping them motivated and active.
“The cool part was the app triggers notifications to the users for upcoming events and we noticed a spike in participation.” – Michael Maassel, Harmony Foundation
Additionally, organizations can use Care Pathway Tools to design structured, milestone-driven experiences. These tools include automated check-ins tailored to specific programs, making it easier for clients to transition smoothly between different levels of care, such as residential to PHP/IOP. This ongoing engagement not only enhances client outcomes but also safeguards revenue streams.
Revenue Protection and New Funding Sources
Engaging alumni can significantly impact an organization’s census, with alumni programming often contributing 30% to 50% of it. Moreover, alumni admissions typically have the lowest cost-per-acquisition compared to other admission sources. CaredFor helps protect revenue by reducing AMA (Against Medical Advice) departures and extending client stays through consistent engagement between clinical sessions.
The platform also creates opportunities for new revenue streams. For instance, organizations can adopt tiered membership models, offering basic access for routine check-ups and premium tiers for expert support or exclusive digital content. This approach generates steady, recurring revenue. Additionally, CaredFor supports remote patient monitoringand telehealth services, which can qualify for reimbursement under existing fee-for-service and value-based care models. Integration with the Welligent EHR further enhances efficiency by syncing appointment data automatically and feeding assessment results directly into client charts, reducing administrative work and streamlining billing processes.
Emerging Trends in Behavioral Health Technology
ACCELERATE 2026 dives into the latest tech developments that empower behavioral health leaders to achieve measurable outcomes. These sessions will showcase how technological advancements are reshaping care delivery. For instance, AI adoption in behavioral health has jumped from 17% to 27%. Organizations using AI-driven clinical insights have reported symptom improvements up to three or four times greater than before.
AI in Predictive Care
AI is playing a growing role in guiding clinical decisions. In early 2026, Guardian Recovery utilized Salesforce‘s AI tools to analyze alumni data and generate readmission risk scores. This allowed them to create prioritized call lists, enabling proactive outreach to individuals at high risk of relapse.
“In the era of fentanyl, one more day for that client out there using because we didn’t appropriately predict their potential relapse is a missed opportunity to help them.” – DJ Prince, Chief Strategy Officer, Guardian Recovery
AI is also transforming treatment plans. “Living” treatment plans, powered by AI, automatically update as symptoms evolve. These plans align SMART goals and interventions in real time using assessment tools like the PHQ-9 or GAD-7. Pathways Recovery Centers, for example, uses wearable biometrics to provide objective clinical evidence. This data has helped secure more covered care days and even negotiate mid-contract rate increases of 20%. Additionally, AI tools are conducting real-time compliance audits, identifying documentation gaps before they lead to denied authorizations.
These AI applications are building the foundation for more integrated and efficient care systems.
Integrated Systems and Interoperability
AI-enhanced decision-making is even more effective when paired with integrated systems that ensure consistent data and streamlined operations. Fragmented platforms – like disconnected EMR, RCM, and CRM systems – can create what’s often called the “Frankenstein effect”, leading to inefficiencies and mistrust in data. To combat this, Guardian Recovery implemented a Power BI infrastructure in early 2026. This system unified data from Salesforce, Kipu, CollaborateMD, and QuickBooks, creating cohesive dashboards. This integration enabled their President to uncover a revenue discrepancy caused by a global rate reset within the first month, rather than four months later, allowing for timely adjustments and recovery before the quarter ended.
“What you get with an integrated system is trust and confidence in the data, so that teams are able to make better decisions and execute on them more quickly.” – Meghan Mouser, VP of Product Management, Kipu Health
ACCELERATE sessions will guide attendees on how to avoid fragmented systems and build unified technology infrastructures that deliver measurable returns.
Why You Should Attend ACCELERATE 2026
ACCELERATE 2026 is the only conference dedicated to exploring tech innovation and AI specifically within the realm of behavioral health. Unlike broader healthcare IT events, this one focuses squarely on the unique challenges faced by behavioral health leaders. Key topics include navigating the final MHPAEA rules, which take effect in January 2026, and preparing for Medicaid changes that could significantly impact revenue streams – potentially in the millions.
Attendees will gain exclusive access to product roadmaps for Welligent EHR, DATIS HCM, and the CaredFor platform. Beyond that, the event offers the chance to connect with peers who are tackling similar operational hurdles. These insights are not just theoretical but practical, offering a pathway to meaningful changes. Whether it’s addressing regulatory updates or overcoming operational bottlenecks, ACCELERATE 2026 provides tools and strategies that can make a real difference.
The value of this conference is evident in real-world examples. For instance, early in 2026, Chris Hunter, CEO of Acadia Healthcare, announced plans to add 500 to 700 new beds, a move projected to increase earnings by $150 million. Similarly, BetterHelp shifted its business model by expanding health insurance coverage to 12 U.S. states and Washington, D.C., transitioning from cash-pay to in-network benefits. This strategic pivot significantly boosted conversion rates. These examples highlight how actionable insights from ACCELERATE 2026 can lead to measurable growth.
Don’t miss out! Register now to take advantage of Early Bird pricing at this link. The knowledge and connections you’ll gain will help you stay ahead of regulatory changes, improve your revenue cycle, and leverage AI solutions to achieve tangible results.
FAQs
Who should attend ACCELERATE 2026?
ACCELERATE 2026 is designed for professionals in behavioral health and healthcare who are eager to gain practical insights, discover the latest product updates, and learn from peer experiences. This event attracts a diverse group, including:
- Clinical leaders focused on patient care and service improvements
- Operational managers aiming to streamline processes and enhance efficiency
- IT professionals working on technology-driven solutions
- Executives dedicated to improving outcomes and workforce strategies
The event offers a mix of workshops, thought leadership sessions, and networking opportunities. It’s the perfect setting for those driving advancements in behavioral health services while navigating the ever-changing healthcare landscape.




