Turnover in behavioral health is expensive and disruptive, impacting finances, patient care, and staff morale. Replacing a single clinician can cost between 30% and 250% of their annual salary, with hidden costs like lost revenue, burnout, and knowledge loss adding to the problem. High turnover rates – 30% to 40% annually – are double those in other healthcare fields, with some organizations seeing rates as high as 70%.
Key takeaways for reducing turnover:
- Retention Programs: Offer career growth opportunities, mentorship, and professional development to keep staff engaged.
- Workplace Culture: Support staff through flexible schedules, open communication, and trauma-informed leadership.
- Workload Management: Use tools like Electronic Health Records (EHR) and automated systems to reduce administrative burdens.
- Technology Solutions: Leverage predictive analytics and Human Capital Management (HCM) systems to identify risks, streamline onboarding, and improve workforce planning.
Organizations that invest in these strategies can reduce turnover costs, improve patient care, and stabilize their workforce. NYC Health + Hospitals, for example, cut behavioral health staff turnover from 18% to 8% by applying data-driven approaches. The solution lies in proactive workforce management and prioritizing staff well-being.
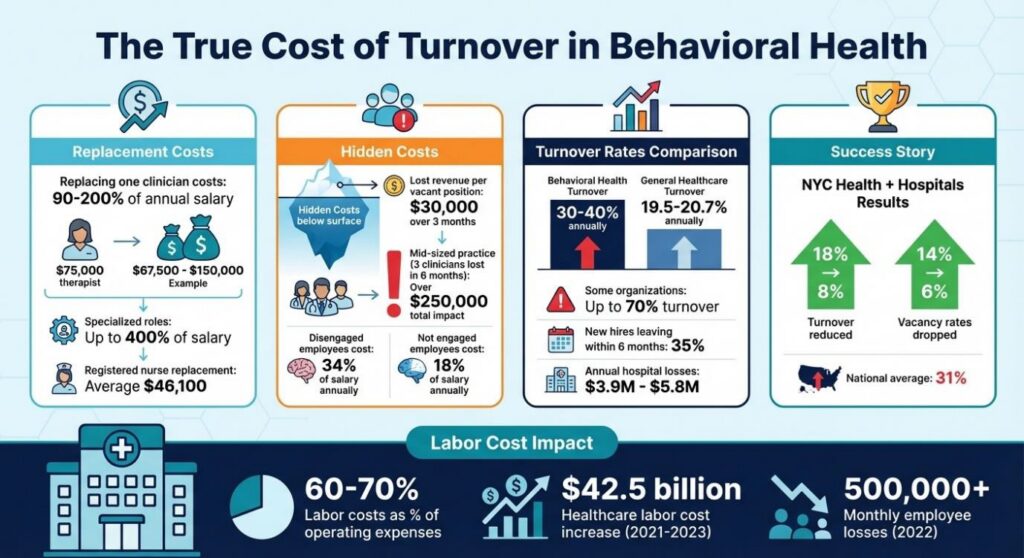
The True Cost of Behavioral Health Turnover: Key Statistics and Financial Impact
The Financial Cost of Turnover in Behavioral Health
Direct Replacement Costs
The moment a clinician leaves, the financial toll begins. Replacing a behavioral health professional typically costs anywhere from 90% to 200% of their annual salary. For instance, replacing a therapist earning $75,000 can cost between $67,500 and $150,000. For specialized roles, the numbers soar even higher – up to 400% of their salary in some cases.
The expenses start piling up right away. Recruitment costs, like job board fees and recruiter commissions (which range from 15% to 25% of the new hire’s salary), are just the beginning. Add in the administrative time spent on screening and interviewing candidates, and the price tag grows quickly. Onboarding is another costly step, with background checks, system setups, and mandatory training adding to the bill. In states like Minnesota, new hires are required to complete 30 hours of training before they can begin working independently.
Then there’s the productivity gap. New clinicians often spend their first 30 to 90 days in training, which means they’re earning a full salary without generating any billable revenue. For example, replacing a registered nurse in a behavioral health setting costs an average of $46,100. These direct costs are just the start – hidden financial burdens make the situation even more challenging.
Hidden Costs of Turnover
What you see on paper is only part of the story. Vacant positions lead to unbillable appointments, costing around $30,000 per clinician over three months. For a mid-sized practice that loses three clinicians within six months, the combined impact of recruitment, lost billing, and administrative strain can exceed $250,000.
The ripple effects don’t stop there. Remaining staff often face increased workloads, leading to burnout and what’s known as “cascading turnover” – a cycle where overburdened employees leave, further compounding the problem . Disengaged employees also take a toll. Actively disengaged workers cost their employer 34% of their salary annually due to lower productivity and absenteeism, while those who are simply “not engaged” still cost 18% . As Bobbi D. Kelly, Director-in-Charge of Talent Advisory at Kreischer Miller, puts it:
“The period between when you fill a position and when that employee becomes efficient enough to make you money is the costliest timeframe in the employment lifecycle”.
Turnover also drains institutional knowledge. When clinicians leave, they take valuable experience and patient relationships with them. In some cases, patients follow their providers to competitors, which can hurt both your reputation and revenue . These hidden costs add up quickly, straining budgets and, more importantly, impacting patient care. Considering that labor costs already make up 60% to 70% of operating expenses in behavioral health, these added financial pressures are hard to ignore.
Turnover Rates in Behavioral Health
The financial burden of turnover reflects a worrying reality: behavioral health professionals leave their roles at much higher rates than others in healthcare. Turnover in this sector ranges from 30% to 40% annually – double the rate seen in other healthcare fields. Some organizations report turnover rates as high as 70%, with about 35% of new hires leaving within their first six months. For comparison, general hospital turnover rates hover between 19.5% and 20.7%.
The range of turnover rates varies widely across roles, with some positions exceeding 70%, further intensifying financial and operational challenges. On a larger scale, hospitals face losses of $3.9 million to $5.8 million annually due to turnover-related expenses. Between 2021 and 2023, healthcare labor costs increased by over $42.5 billion, and in 2022 alone, the U.S. healthcare industry lost more than 500,000 employees each month. The pressure to manage these costs is only growing.
NWI Webinar 57: Beyond Burnout: Transforming Organizations and Systems to Reduce Workforce Turnover
How Turnover Affects Operations and Patient Care
Turnover creates challenges that extend far beyond just financial losses. When behavioral health professionals leave, the effects ripple through the organization, impacting patients, staff, and leadership alike.
Disrupted Patient Care and Therapeutic Relationships
In behavioral health, the connection between a patient and their provider is at the heart of effective treatment. When a clinician leaves, patients often have to start over, which is the point where drop-off rates are the highest. This issue becomes even more complicated when care is fragmented across multiple providers or billing systems. Patients who lose consistent outpatient or community-based care after being discharged from the hospital often have no choice but to turn to emergency or inpatient services for stabilization – services that are not designed for long-term therapeutic care.
Adding to the challenge, data from 2009–2010 revealed that only 55% of psychiatrists accepted private insurance, compared to 89% of other medical specialists. This makes it significantly harder for patients to find new providers when their current one leaves. To address these challenges, New Mexico introduced a “Treat First” model between 2015 and 2024. This approach allowed patients to receive immediate clinical treatment with a provisional diagnosis during their first four visits. The results? Better provider capacity, improved access to care, greater patient satisfaction, fewer no-shows, and reduced burnout among staff. However, when clinicians leave, the disruption to care continuity often increases workloads for the remaining team.
Higher Workload and Burnout Among Remaining Staff
When a clinician leaves, their caseload doesn’t disappear – it gets redistributed to the remaining staff. This added workload leads to longer waitlists, shorter patient sessions, and more administrative responsibilities, pulling clinicians further away from the core of their work: patient care. It’s no surprise that nearly half of behavioral health workers are considering leaving their roles or even the field altogether.
The loss of colleagues can take a toll on morale and job satisfaction, creating a cycle of burnout. Outdated processes and redundant paperwork only add to the frustration, often forcing staff to take on tasks below their professional licensure levels just to keep things running
These operational challenges inevitably trickle up, placing even more pressure on HR teams and leadership.
Added Pressure on HR and Leadership
Turnover doesn’t just disrupt day-to-day operations – it creates significant challenges for HR and leadership. From managing temporary staff and overtime schedules to keeping services operational despite vacancies, the strain is immense. Supervisors, many of whom are promoted for their clinical expertise rather than management skills, often struggle with team communication and fostering a sense of psychological safety.
As the National Council for Mental Wellbeing highlights:
“Leadership is one of the strongest predictors of workforce stability. But many supervisors are promoted for clinical skill, not leadership prowess” .
Frequent turnover not only makes it harder for organizations to scale and grow but can also damage their reputation. This, in turn, discourages new patients from seeking care and limits revenue potential. For HR leaders, the task isn’t just about filling vacancies – it’s about rethinking systems to break the turnover cycle before it erodes the organization’s foundation.
How to Reduce Turnover in Behavioral Health
Reducing turnover in behavioral health starts with addressing the underlying reasons why staff leave. Organizations that prioritize retention not only improve staff satisfaction but also enhance patient care. Strategies like career development, workload management, and fostering a supportive culture can make a significant difference.
Build Retention Programs and Career Paths
Retention begins with creating pathways for growth and support within your organization. Programs like mentorship and peer support help new hires feel connected and encourage long-term commitment . Developing internal talent pipelines can ease recruitment pressures while promoting a culture of growth.
Offering paid time for professional development is another key step. This approach allows clinicians to stay engaged and refine their skills without overloading their schedules. For instance, the Illinois Behavioral Health Workforce Center provides a “Retention Toolkit” to help leaders combat burnout and secondary trauma. Tools like the Organization Retention Assessment can also help identify areas of dissatisfaction before they escalate into turnover.
“A stable and consistent workforce is pivotal to maintaining a high standard of care, ensuring that patients have continuity in their treatment.” – Harris Integrative
Create a Better Workplace Culture
Beyond career development, a supportive workplace culture is critical for retention. Trauma-informed leadership plays a central role here, as it acknowledges the secondary trauma employees face daily. Leaders who provide constructive feedback and help align tasks with employees’ career goals create a more supportive environment.
Flexible scheduling and family-friendly policies can also improve work-life balance. Encouraging open communication allows staff to express challenges without fear of judgment. Employees who feel valued – especially those with lived experience in behavioral health – are more likely to stay. A workplace culture built on belonging and shared purpose can be a powerful retention tool.
Manage Workloads and Provide Staff Support
Heavy workloads are a common issue in behavioral health, but they can be managed with the right tools and strategies. Specialized Electronic Health Records (EHR) and automated billing systems can significantly cut down on administrative tasks. By streamlining these processes, staff can spend more time on meaningful clinical work.
Fair workload distribution is equally important. Regularly reviewing compensation to ensure it aligns with market rates for your area and experience levels is another way to show staff they’re valued. Offering robust Employee Assistance Programs (EAPs), ample paid time off, and clear paths for advancement further demonstrates leadership’s commitment to reducing stress and supporting their team.
“Effective staff retention is essential for delivering quality care and reducing the challenges of turnover.” – Behavioral Health Workforce Center
Using Technology to Manage and Keep Staff
Technology gives HR teams a powerful way to tackle employee turnover and strengthen retention strategies. The right tools transform scattered workforce data into actionable insights, automate repetitive tasks, and foster stronger connections between employees and their work.
Using Workforce Data to Predict Turnover
Predictive analytics can help identify employees at risk of leaving – even before they submit their resignation. Machine learning models analyze data like absenteeism, engagement levels, workload, and performance trends to flag potential issues. For example, a study involving 303 employees at community behavioral health organizations found that machine learning models trained on HR data predicted turnover with 0.63 accuracy. When factors like career advancement opportunities, expectation alignment, and supervision quality were added, accuracy rose to 0.76 .
NYC Health + Hospitals demonstrated the impact of data-driven workforce strategies. By implementing these methods, they reduced behavioral health staff turnover from 18% in 2022 to just 8%, far below the national average of 31%. Vacancy rates also dropped from 14% to 6%. Since January 2024, the organization has hired around 100 new psychiatrists, nearly 20 psychiatric nurse practitioners, and over 400 social workers. Dr. Omar Fattal, Chief of Behavioral Health Services, shared that the system is gaining a reputation as an “employer of choice in public behavioral health”, with more applications and faster hiring processes. This approach highlights how integrated systems can effectively manage the employee lifecycle.
Human Capital Management (HCM) Systems
HCM platforms like ContinuumCloud‘s DATIS streamline every stage of the employee lifecycle, from payroll and performance tracking to onboarding and compliance management. Behavioral health organizations benefit from features like credential tracking and position control, which ensure staff maintain necessary licenses and align staffing with budget needs.
These systems also address common retention challenges by tracking career progression, analyzing pay equity, and identifying skill gaps before they lead to dissatisfaction. Research shows that perceived fairness in compensation has a stronger influence on retention than salary alone.
For instance, Behavioral Progression, Inc. cut onboarding time for therapists from four weeks to just 2.5 weeks by automating manual processes with HCM templates. Their HR team handled tasks three times faster, and new hires asked 60% fewer questions during onboarding. Similarly, All About Kids, a pediatric therapy provider with 1,200 employees, eliminated documentation errors and improved manager oversight by switching from a paper-based system to an automated one.
Scheduling and Communication Tools
EHR platforms with built-in scheduling tools can reduce administrative workloads by 30-50%. AI-powered scheduling ensures balanced workloads, helping to prevent burnout – a problem that can cost organizations 15-20% of payroll annually. Mobile tools that allow employees to view schedules, swap shifts, and request time off in real time enhance work-life balance.
Communication platforms also play a key role by creating channels for employees to share concerns before they escalate. Among 14 companies with 184,715 employees, those who used evidence-based mental health benefits saw an 11% turnover rate within 12 months compared to 22% for those who didn’t. Combining wellness tools with better scheduling can deliver up to 425% ROI in retention. By integrating these technologies, HR teams can more effectively support their staff and reduce turnover, aligning with broader retention strategies discussed earlier.
Conclusion
Behavioral health turnover is expensive, costing anywhere from 30% to 150% of an employee’s annual salary. But the financial hit doesn’t stop there – turnover also brings overtime expenses, reduced productivity, and a loss of institutional knowledge that’s hard to replace.
The ripple effects of turnover impact every corner of an organization, from financial health to operational efficiency and, most importantly, patient care. That’s why it’s essential to focus on solutions that address the underlying causes. Offering career growth opportunities, creating supportive workplace cultures, and balancing workloads are just a few ways to tackle these challenges head-on. In fact, nearly 48% of employees say they’re more likely to stay with organizations that actively listen to and act on their feedback. This makes it clear: retention strategies aren’t just nice to have – they’re a must.
Technology also plays a key role. Tools like predictive analytics and HCM systems, such as ContinuumCloud’s DATIS, can simplify onboarding, cut down on administrative tasks, and improve workforce planning . The cost of doing nothing is steep. With behavioral health turnover rates averaging 40% – and sometimes spiking as high as 70% – inaction only fuels cycles of understaffing and burnout. By prioritizing retention, organizations can avoid the much higher costs of constant recruitment and training.
The way forward is clear: move from reactive crisis management to strategic workforce planning. Calculate the real costs of turnover, identify problem areas, and use the right tools to build a more stable and engaged team.
FAQs
How do I calculate the true cost of turnover for my organization?
To figure out turnover costs, you need to factor in both direct expenses and indirect costs. Direct expenses include things like recruiting, hiring, and onboarding new employees. Indirect costs, on the other hand, cover areas such as lost productivity, a decline in institutional knowledge, and potential impacts on patient care. Beyond these, there are also harder-to-quantify effects, like disruptions to service.
For instance, turnover rates in behavioral health can reach as high as 40%, which can lead to a noticeable rise in costs. By understanding the reasons employees choose to leave, you can develop strategies to manage and lower these expenses.
What are the fastest ways to reduce clinician burnout and workload?
Which HR metrics best predict who is likely to quit next?
Understanding why employees leave is crucial in behavioral health, where turnover can disrupt care and impact team morale. Key metrics to watch include employee engagement, workload, burnout levels, and the overall quality of the work environment.
How can you track these factors? Tools like staff surveys, absenteeism rates, and exit interviews offer valuable insights into dissatisfaction and stress levels. For example, high absenteeism or recurring complaints in exit interviews might signal larger workplace issues.
It’s also important to monitor specifics like workload distribution, scheduling flexibility, and participation in professional development opportunities. These areas often reveal employees who feel overburdened or undervalued – both common reasons for leaving.
By combining employee feedback with hard data on engagement and stress, HR teams can better identify patterns and predict which team members might be at risk of leaving next. This proactive approach helps address problems before they escalate.




