Behavioral health organizations often face challenges when selecting the right platform for their needs. General healthcare systems, while popular, fall short in addressing the unique requirements of behavioral health programs, such as long-term care, group therapy, and compliance with strict regulations like 42 CFR Part 2. Specialized platforms, like ContinuumCloud‘s Welligent, are purpose-built to handle these demands efficiently. Here’s why choosing the right system matters:
- General Platforms: Designed for short-term, acute care, they lack tools for residential programs, group therapy documentation, and behavioral health-specific reporting.
- Specialized Platforms: Tailored for behavioral health, they streamline clinical workflows, reduce documentation time, and ensure compliance with regulations like 42 CFR Part 2.
Key Takeaways:
- Efficiency: Specialized platforms save time with features like AI-powered clinical notes and real-time compliance checks.
- Compliance: Behavioral health platforms handle stricter privacy rules for SUD records.
- Scalability: Tools like Welligent’s modular design grow with your organization, supporting multiple care levels and programs.
Choosing a platform tailored to behavioral health ensures smoother operations, better compliance, and the ability to scale services effectively.
1. ContinuumCloud‘s Welligent

Let’s take a closer look at how Welligent addresses the unique challenges of behavioral health with its tailored features.
ContinuumCloud’s Welligent is a cloud-based platform designed specifically for behavioral health workflows, accessible from any device. Unlike general healthcare systems, it caters to a wide range of care levels – covering inpatient and residential treatment, Intensive Outpatient Programs (IOP), and Medication-Assisted Treatment (MAT). Beyond addiction treatment, it also supports foster care agencies, Intellectual and Developmental Disabilities (IDD) organizations, and public health entities.
Support for Multiple Levels of Care
Welligent is built to handle the unique needs of both residential and outpatient programs. It enables organizations to manage IOP, residential, and MAT programs all within a single system, removing the hassle of juggling disconnected tools or spreadsheets. This unified approach simplifies clinical documentation, a cornerstone of behavioral health workflows.
Behavioral Health-Specific Clinical Documentation
Documentation is one of the biggest time drains for behavioral health providers, consuming anywhere from 34% to 55% of their work hours. Welligent tackles this issue with AI-powered tools like Clinical Notes AI, which listens to sessions and drafts clinical notes automatically. In 2024, organizations like Coleman Health Services and GRAND Mental Healthreported impressive results: a 70% reduction in documentation time, faster note submissions (from five days to just 1.5 days), and over 400 staff hours saved. Additionally, more than 80% of progress notes were completed automatically.
The platform ensures compliance with regulatory and payer standards by maintaining the “Golden Thread”, which aligns diagnoses, treatment plans, and session notes automatically. For group therapy, its specialized AI summarizes group discussions into concise notes for both the group and individual participants.
“Our clinical staff have found the integration of Eleos into Welligent simple and efficient.” – Susan Blue, CEO, Community Services Group
Welligent also includes a mobile app with offline functionality, letting clinicians document care in the field without internet access. Once connectivity is restored, notes sync automatically. Its “Comply” feature performs real-time audits on all documentation, flagging potential issues before submission. One organization saw a 40% reduction in payer reviews for level of care placement after adopting this feature. These tools directly address the documentation inefficiencies that burden providers.
Operational Visibility and Reporting
Welligent provides custom dashboards that offer real-time insights into outcomes, productivity, and compliance. The platform tracks clinician productivity, monitors staff activity, and flags documentation compliance issues automatically. For financial management, its integrated revenue cycle tools handle real-time eligibility checks, automated claims processing, and create exportable reports tailored for funders and auditors.
When paired with DATIS e3 HCM (available as an add-on), Welligent expands its capabilities to include workforce analytics, covering payroll, timekeeping, and resource allocation. This integration creates a “single source of truth” for workforce management, enabling organizations to allocate resources efficiently across various programs and locations.
Scalability for Growth
Welligent’s modular design allows organizations to expand their capabilities as they grow. The core platform includes clinical documentation, billing dashboards, and reporting tools, while additional modules – like CaredFor for patient engagement or the DATIS e3 integration for workforce management – can be added as needed. This flexibility ensures that organizations can scale their operations seamlessly.
2. General Healthcare Platforms
Behavioral health organizations often start with general healthcare platforms because of their widespread use and established reputation. However, these systems are primarily designed for short-term, acute care scenarios – like hospital stays, surgeries, or emergency visits. This focus on episodic treatment doesn’t translate well to behavioral health, which relies on ongoing, multidisciplinary, and program-focused care models. These key design mismatches highlight why traditional platforms often fall short in meeting the needs of behavioral health services.
Support for Multiple Levels of Care
General healthcare systems frequently lack the tools needed to manage the diverse care levels found in behavioral health programs. Features like ASAM criteria, DSM-5 coding, and workflows for residential care or outpatient services (such as Partial Hospitalization Programs or Intensive Outpatient Programs) are often missing. This forces organizations to either juggle multiple systems or resort to manual workarounds, creating fragmented care delivery. These limitations also extend to clinical documentation, posing additional challenges.
Behavioral Health-Specific Clinical Documentation
Documentation processes in general platforms are typically built around ICD-10 codes and traditional medical models, which don’t align with the psychosocial or problem-goal-objective-intervention frameworks used in behavioral health. For example, group therapy – a cornerstone of many behavioral health programs – often requires clinicians to write separate notes for each participant, adding unnecessary administrative burdens. Studies have shown that these inefficient documentation practices significantly impact operations.
Another critical issue is compliance with 42 CFR Part 2, which imposes stricter rules for managing substance use disorder records compared to standard HIPAA regulations. Many organizations only discover these compliance gaps after implementation, when they encounter billing or operational hurdles.
Operational Visibility and Reporting
General healthcare platforms often focus their reporting features on metrics like vitals and acute care outcomes, leaving behavioral health-specific needs unmet. Tools such as PHQ-9, GAD-7, or C-SSRS, which measure behavioral health outcomes, are rarely integrated. As a result, leadership teams frequently resort to exporting raw data and manually compiling reports to track key metrics like program census, staff productivity, or documentation compliance.
Scalability for Growth
While general platforms can technically scale, the costs and complexities of customization often outweigh the benefits. For instance, implementing an enterprise-level healthcare platform can cost over $100,000, with rollout timelines ranging from 6 to 18 months. As organizations grow – adding new programs or locations – these complexities only multiply. On the other hand, behavioral health-specific platforms typically charge between $200 and $500 (or more) per provider each month. These systems often offer a lower total cost of ownership by reducing inefficiencies and eliminating the need for workarounds.
Advantages and Disadvantages
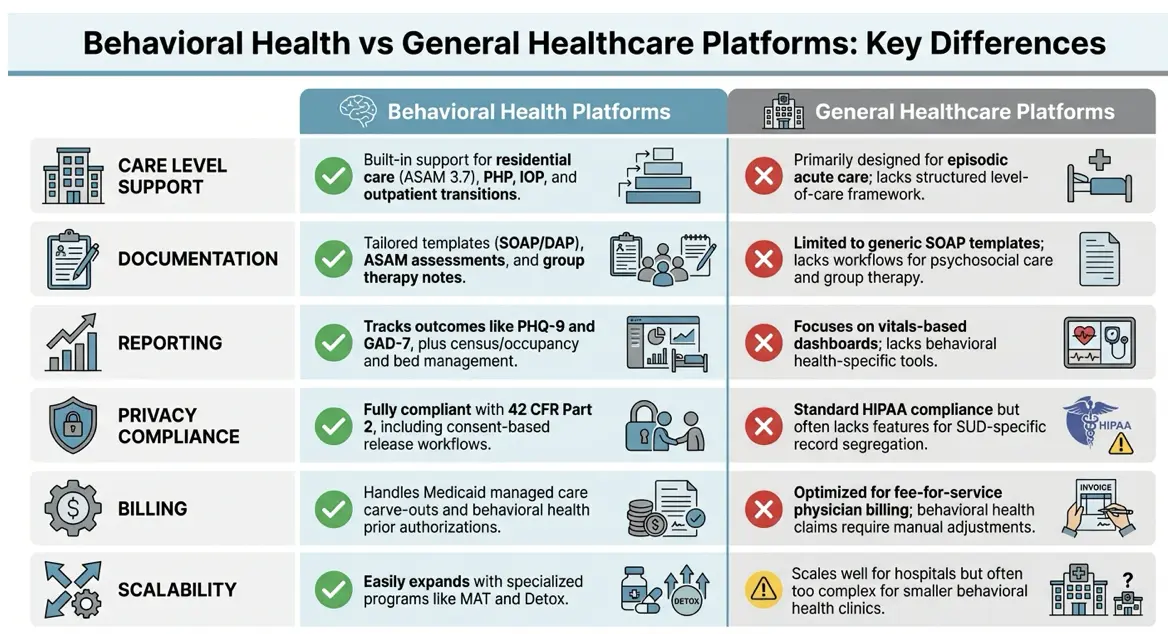
Expanding on earlier operational challenges, it’s clear that the choice of platform significantly impacts behavioral health organizations. The table below provides a side-by-side comparison of behavioral health–specific platforms and general healthcare platforms, focusing on the features that matter most.
|
Feature |
Behavioral Health–Specific Platforms |
General Healthcare Platforms |
|
Care Level Support |
Built-in support for residential care (ASAM 3.7), PHP, IOP, and outpatient transitions. |
Primarily designed for episodic acute care; lacks a structured level-of-care framework. |
|
Documentation |
Offers tailored templates (SOAP/DAP), ASAM assessments, and group therapy notes. |
Limited to generic SOAP templates; lacks workflows for psychosocial care and group therapy. |
|
Reporting |
Tracks outcomes like PHQ-9 and GAD-7, plus census/occupancy and bed management. |
Focuses on vitals-based dashboards; lacks behavioral health–specific tools for tracking outcomes. |
|
Privacy |
Fully compliant with 42 CFR Part 2, including consent-based release workflows. |
Standard HIPAA compliance but often lacks features for SUD-specific record segregation. |
|
Billing |
Handles Medicaid managed care carve-outs and behavioral health prior authorizations. |
Optimized for fee-for-service physician billing; behavioral health claims require manual adjustments. |
|
Scalability |
Easily expands with specialized programs like MAT and Detox. |
Scales well for hospitals but often too complex for smaller behavioral health clinics. |
These distinctions directly influence daily operations, efficiency, and costs. Behavioral health platforms are purpose-built to align with the workflow of treatment, from the initial ASAM assessment to discharge planning. This alignment eliminates the need for heavy customization, which is often required with general healthcare systems. For example, general platforms struggle to efficiently support group documentation, a critical component of behavioral health care.
Cost is another critical factor. While general platforms may seem more affordable upfront, they often involve high initial fees and long implementation timelines. In contrast, behavioral health platforms typically operate on predictable monthly subscriptions, minimizing unexpected costs. They also reduce billing complications and administrative inefficiencies, which can lead to revenue loss over time.
Additionally, behavioral health platforms simplify compliance with 42 CFR Part 2 regulations, automatically managing the complexities of consent-based workflows. By understanding these differences, behavioral health organizations can make informed technology choices that align with their operational needs.
Conclusion
Choosing the right platform for residential and outpatient behavioral health isn’t just about picking the right technology – it’s a strategic move that impacts the way care is delivered at every level. Welligent is specifically designed to handle the long-term, multidisciplinary needs of behavioral health, unlike general healthcare systems, which focus on short-term, acute care and often fall short of meeting the unique requirements of behavioral health services.
Specialized platforms help organizations avoid expensive workarounds, ease documentation with templates tailored for behavioral health, and ensure compliance with 42 CFR Part 2 without relying on manual processes.
To maximize these advantages, it’s crucial to evaluate how well a platform fits into existing workflows. Engaging clinicians early in the process can help ensure the system reduces their workload rather than adding to it. Test how well client records move between residential and outpatient care to ensure smooth transitions. Additionally, ask vendors to show how they handle the segregation of substance use records and log consent-based disclosures to meet 42 CFR Part 2 requirements.
For organizations managing multiple programs, scalability is key. Welligent’s unified system eliminates data silos, making it easier to expand services and meet growing demands without sacrificing efficiency.
FAQs
How do I know if my organization needs a behavioral health-specific platform?
What should I ask vendors to prove 42 CFR Part 2 compliance?
Additionally, ask whether the vendor has obtained independent security certifications like SOC 2 or HITRUST, which indicate robust data protection measures. It’s also a good idea to request detailed workflows outlining how the system handles patient authorizations and enforces data-sharing restrictions. This can help confirm the platform aligns with confidentiality requirements.
How can I evaluate whether the system supports smooth residential-to-outpatient transitions?
To make the shift between residential and outpatient care as seamless as possible, prioritize platforms with integrated workflows. These should enable shared clinical documentation, connect treatment plans directly to clinical goals, and make session notes easily accessible across different programs. Additionally, look for systems equipped with reporting tools that help monitor program capacity, utilization rates, and client transitions.
A unified system like this doesn’t just cut down on administrative tasks – it also improves care coordination and ensures consistent support for clients across both residential and outpatient services.




